Health
New Covid vaccine arrives first in West Wales
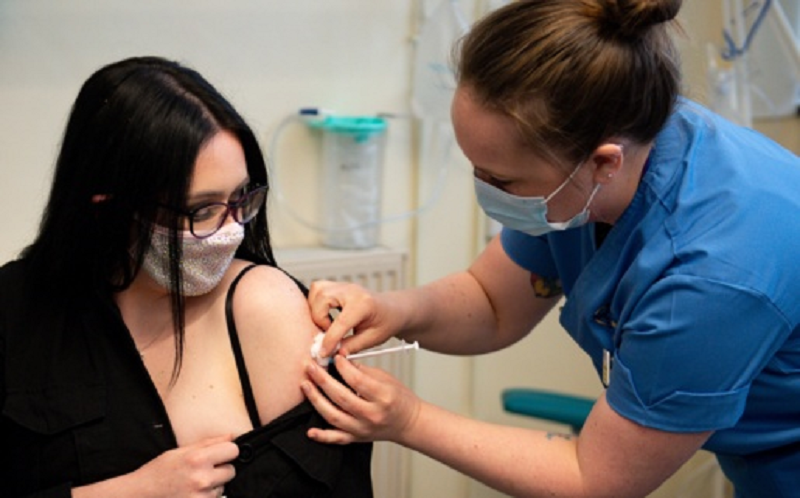

HEALTH BOARD ‘DELIGHTED’
The Medicines and Healthcare Products Regulatory Agency (MHRA) authorised the Moderna vaccine as safe and effective in January 2021 following rigorous clinical trials.
Moderna is the third Covid-19 vaccine distributed in the UK.
Two other vaccines, the Pfizer vaccine and the Astra Zeneca vaccine, are already in use across the UK. 31 million people across the UK have received their first shot of one of those vaccines since the inoculation programme began in December last year.
Supplies arrived in Wales on Tuesday, April 6.
5,000 doses were delivered to vaccination centres in the Hywel Dda University Health Board area.
The Moderna vaccine is a two-dose vaccine given at an interval of between four and twelve weeks.
Ros Jervis, Director of Public Health for Hywel Dda University Health Board, added: “We’re delighted to be able to use the Moderna vaccine for deployment across west Wales.
“We will be using this new vaccine, alongside Oxford Astra-Zeneca, to continue the immunisation’s roll out to our communities in Carmarthenshire, Ceredigion and Pembrokeshire.
“We are incredibly lucky to have a third vaccine in Wales, with a long shelf life and the ability to be easily transported, to help deliver the vaccination programme to small clinics across our rural communities.”
THE MODERNA VACCINE EXPLAINED
The Moderna vaccine does not contain the virus to produce immunity.
It cannot give you COVID-19.
The injection stimulates the body’s natural defences (immune system). It works by making the body produce its own protection (antibodies) against the virus that causes the COVID-19 infection.
The vaccine delivers the ‘instructions’ that cells in the body can use to make antibodies to fight the virus that causes COVID-19.
As with any vaccine, Moderna may not fully protect all those who receive it. Those who get it may not be fully protected until two weeks after the vaccine’s second dose.
In trials, the vaccine was 94.1% effective in preventing Covid-19 infection in patients with no prior history of the disease. It was 100% effective in preventing patients from developing the severe Covid-19 symptoms that lead to hospitalisation.
Although the Moderna vaccine is the priciest of the vaccines yet rolled out, it has an advantage over the Pfizer vaccine. It can be stored in a regular fridge for up to fourteen days after its delivery to a vaccination centre.
It contains no ingredient derived from animals.
A KEY MILESTONE
Health Minister Vaughan Gething said: “This is another key milestone in our fight against the COVID-19 pandemic. The third vaccine for use in Wales significantly adds to our defences in the face of coronavirus. It will help to protect our most vulnerable.
“Every vaccine given to someone in Wales is a small victory against the virus, and we would encourage everyone to go for their vaccine when invited.
“If people cannot attend their appointment, we ask them to let the health board know via the contact details provided in their invitation as this vaccination slot can be offered to someone else rather than be wasted.
“Once you have been vaccinated, you should continue to follow guidance, staying two metres apart, washing your hands and wearing a face covering to protect those around you.
“I want to thank all those who have been working tirelessly to deliver the vaccine across Wales and help us meet our second milestone of offering a vaccine to all phase one priority groups. I also want to thank the 1.5 million people in Wales that have already come forward for their vaccine and done their bit in this national effort.”
Welsh Conservative deputy health spokesperson and candidate for Ceredigion and Mid and West Wales, Amanda Jenner, said: “The Conservative UK Government’s decision to go it alone has been fully vindicated with the phenomenal results of the British vaccination programme.
“The roll-out of the Moderna vaccine, administered by our outstanding NHS and volunteers, will boost our ability to protect Welsh people and restore our freedoms.”

VACCINE SUPPLIES
Starting from the middle of last year, the UK Government secured a deliberate oversupply of vaccine to ensure continuity of supply.
As part of that strategy, the Department of Health placed provisional orders – pending approval by the medicines’ regulator – of seven different vaccines in different stages of development.
The UK has ordered 40 million doses of Pfizer’s vaccine, 100 million doses of the Oxford vaccine, and 17 million doses from Moderna.
A further four vaccines are either in clinical trials or awaiting MHRA approval: Novavax (60 million doses, Janssen (30 million doses), Valneva (60 million doses), GlaskoSmithKline (60 million doses).
The number of Covid-19 vaccine doses on order is enough to fully inoculate the UK’s entire population twice.
We will have offered a first dose of the vaccine to all those in priority groups 5-9 by Sunday 18 April.
To ensure no one is left behind, this week the health board has launched an appeal asking people in groups 1 to 9 who have not been contacted to get in touch to arrange their first vaccine dose.
If one or more of the following applies to you and you have not received your first vaccine appointment, please contact the health board on 0300 303 8322 or by email [email protected].
- are aged 50 or over
- are aged 16 to 64 and have underlying health conditions that put you at increased risk of COVID-19 mortality
- work in a care home or in health and social care in Carmarthenshire, Ceredigion or Pembrokeshire
- are the primary unpaid carer of an elderly or disabled adult who is at increased risk of COVID-19 mortality, or a child with severe neuro-disabilities
THE SECOND DOSE
Second doses are essential for longer-term protection, so it’s important that everyone comes forward for their full course when called.
When you will be contacted for your second vaccine dose depends on which vaccine you have received.
We are asking anyone who received the Pfizer vaccine and has not received a second vaccine appointment yet, to get in touch as soon as possible on 0300 303 8322. Please note our phone lines get very busy at times and you may have to wait for the call to be answered. You can also contact us by emailing your name and contact phone number to [email protected].
The health board aims to complete all second Pfizer vaccine doses by week commencing Monday 12 April.
To check which vaccine you received, look at the card given to you when you received your first vaccine. It will say if you received either the Pfizer BioNtech vaccine or the Oxford AstraZeneca vaccine.
If you received a first vaccine dose of the Oxford AstraZeneca vaccine, we politely ask that you do not contact your GP practice or health board at this time to ask about a second vaccine appointment. You will be contacted when it is your turn for a second dose – we are calling those who received a Pfizer first dose at this time.
Care home residents, people aged over 80 and all other priority groups who have received the Oxford AstraZeneca vaccine at the GP surgery will be contacted between 11 to 12 weeks following their first vaccine with an appointment time.
Confidence is building around the effectiveness of the vaccines.
UK and EU regulators have also been very clear about the safety of the vaccines. The benefits of vaccination far outweigh any possible risks.
Health
Davies and Kurtz accuse Welsh Government of ‘passing the buck’ over Hywel Dda plans

Concerns grow over Withybush services as ministers insist decisions rest with health board
THE WELSH GOVERNMENT has been accused of “ducking responsibility” and “hiding behind an unelected health board” amid growing concern over proposed NHS service changes in west Wales.
Samuel Kurtz MS and Paul Davies MS have criticised ministers following a formal response to their joint letter raising alarm about plans linked to Hywel Dda University Health Board’s Clinical Services Plan (CSP), which was approved at an extraordinary meeting in February.
The plan outlines significant changes to how services are delivered across the region, with implementation expected to begin in the next Senedd term and continue over several years.
In a reply dated March 26, Cabinet Secretary for Health and Social Care Jeremy Miles confirmed that responsibility for planning and delivering NHS services lies with local health boards, adding that decisions on the CSP “rest with the health board.”
He also sought to reassure concerns about Withybush Hospital, stating that emergency department services were not included in the CSP decision.
However, the response has drawn sharp criticism from local politicians, who argue that the Welsh Government cannot distance itself from decisions affecting frontline care.
Paul Davies said: “This response is deeply disappointing but sadly not surprising. The Welsh Government is once again trying to pass the buck and avoid accountability by hiding behind an unelected health board.
“Let’s be absolutely clear – health boards are not independent actors. They are created, funded and directed by the Welsh Government. Ministers cannot wash their hands of decisions that will have such a profound impact on communities across west Wales.”
Samuel Kurtz echoed those concerns, warning that public confidence is being eroded.
“People in Pembrokeshire are rightly concerned about what these changes mean for local services, particularly at Withybush Hospital,” he said.
“Attempting to suggest that key services like the emergency department sit outside of these plans will do little to reassure the public, when we have seen services hollowed out and destabilised over the last decade.
“The Welsh Government must stop hiding behind process and start taking responsibility for the future of healthcare in our communities.”
The Herald understands that concerns remain widespread among residents and campaigners, particularly over the long-term future of hospital services in Pembrokeshire, with fears that centralisation could lead to longer travel times for urgent care.
Hywel Dda University Health Board has previously said the changes are designed to improve safety, sustainability and outcomes for patients, but the proposals continue to generate strong local opposition.
Health
Mental health referrals shake-up as 111 service rolled out across west Wales

Concerns raised over phone-based support replacing GP referrals
ADULTS seeking routine mental health support in west Wales will increasingly be directed to a telephone helpline instead of face-to-face services, following a major decision by Hywel Dda University Health Board.
The Health Board has approved a permanent change to how patients in Ceredigion access support, with plans to roll out the same system across Pembrokeshire and Carmarthenshire in phases.
Under the new pathway, patients assessed by their GP as needing non-urgent mental health support will be told to contact the NHS 111 Wales “Press 2” service, rather than being referred to community mental health teams.
The change was first introduced in Ceredigion in March 2025 as an emergency response to staff shortages.
Health chiefs now say the model has proven “safe and effective,” claiming it allows patients to receive quicker support while freeing up specialist teams to deal with more serious cases.
Liz Carroll, the Health Board’s Service Director for Mental Health and Learning Disabilities, said: “Making this change permanent will mean more adults needing non-urgent support will access help much quicker.”
She added that the move would also create capacity for those with “more complex or urgent mental health needs.”
Concerns over access and understanding
Despite the positive assessment, the decision follows a nine-week consultation in which concerns were raised by patients and professionals.
Feedback highlighted confusion about how the 111 Press 2 service works, what support it can offer, and its limitations.
There were also worries about accessibility for people who struggle with telephone-based services, as well as questions around medication and prescribing.
Andrew Carruthers, Chief Operating Officer at the Health Board, acknowledged the concerns.
He said: “People told us they wanted greater clarity and consistency… and highlighted gaps in understanding about 111 Press 2.”
He added that steps would be taken to improve awareness and build trust as the system is rolled out more widely.
Shift driven by pressure on services
Before the change, some patients in Ceredigion faced waits of up to 28 days or more for a face-to-face assessment.
However, data suggested that fewer than five per cent of those referred required that level of specialist input.
Health officials say diverting less urgent cases to the 111 service has improved access times and allowed community mental health teams to prioritise higher-risk patients.
The Health Board also confirmed there has been no increase in serious incidents or complaints linked to the temporary system.
What it means for Pembrokeshire
The phased rollout means patients in Pembrokeshire will soon see similar changes when seeking help for non-urgent mental health issues.
GPs will still be able to refer patients directly to specialist teams where cases are urgent or complex.
The NHS 111 Wales Press 2 service operates 24 hours a day and offers free access to mental health support, including Welsh-language provision.
However, the shift marks a significant move away from traditional GP-led referrals — and is likely to prompt debate over whether remote access can fully replace in-person care.
Health
GP crisis driving NHS pressure in Wales, Senedd report warns
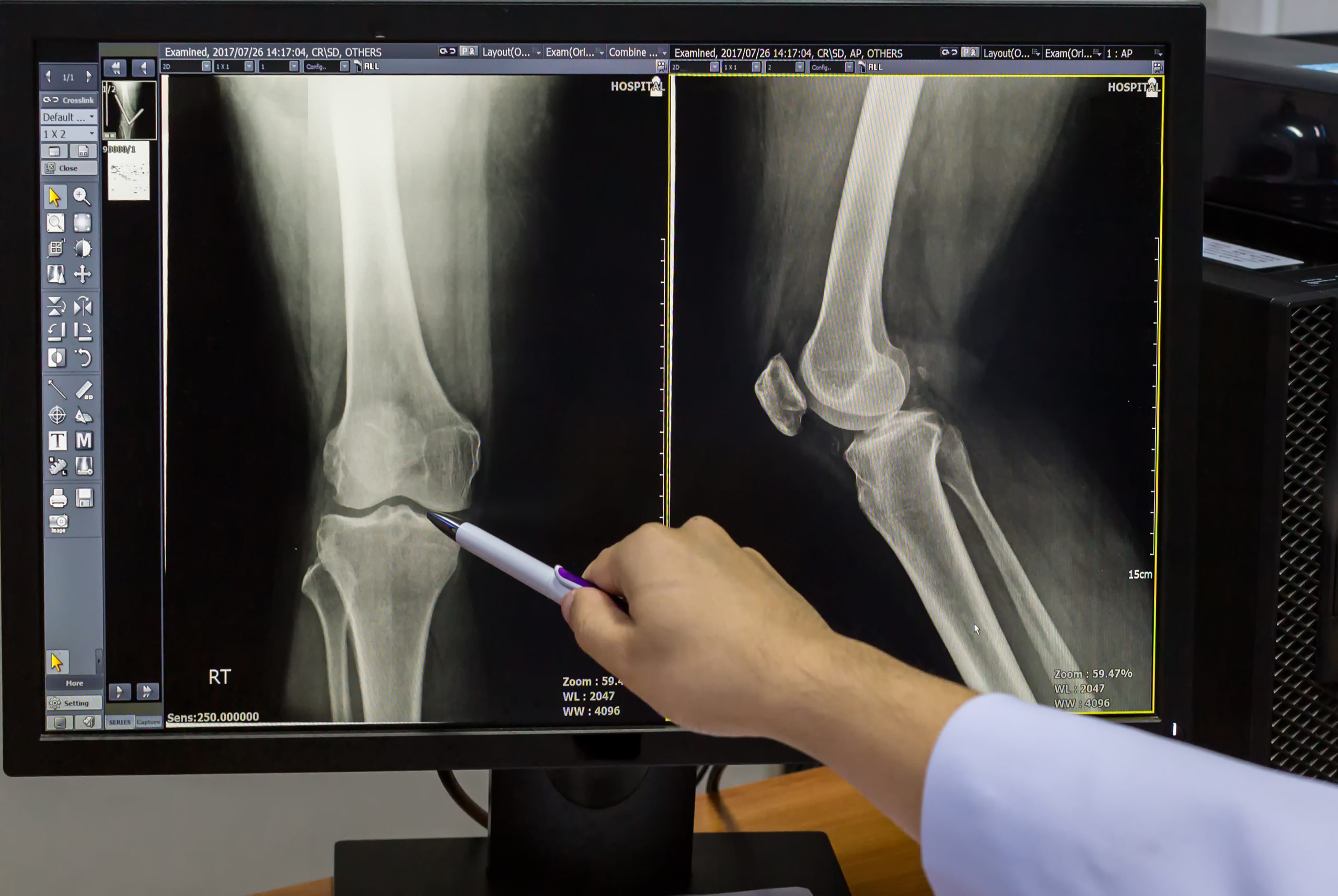
Falling GP numbers and funding gaps blamed for worsening hospital delays
THE NHS crisis highlighted earlier this week is being driven in part by a deepening shortage of GP services, a new Senedd report has revealed.
As previously reported by The Herald, politicians have raised serious concerns about mounting pressure on hospitals, long waits in A&E, and the growing strain on frontline services. Now, a report published on Friday (Mar 27) by the Senedd’s Health and Social Care Committee points to the root of the problem — a weakening primary care system.
The Committee warns that without urgent investment in GP services and preventative care, demand across the NHS will continue to rise beyond capacity.
Sharp decline in GP practices
The report highlights a long-term fall in the number of GP practices across Wales.
In 2002, there were 516 practices operating nationwide. By the start of the pandemic in 2020, that number had dropped to 404. Today, just 374 remain.
The decline has been felt most acutely in rural areas, including west Wales, where fewer practices are now expected to serve growing populations with increasingly complex health needs.
The result, the report suggests, is more patients turning to already overstretched hospital services.
Funding model under pressure
Despite Welsh Government commitments to prioritise community healthcare, the Committee heard evidence that funding has not kept pace with demand.
Concerns were also raised about the current funding formula used for GP practices, which critics say fails to properly reflect deprivation, illness levels and the challenges of delivering care in rural areas.
Without reform, the Committee warns that general practice risks becoming unsustainable, with inequalities in access likely to widen.
Access frustration growing
Patients across Wales continue to face difficulties accessing GP appointments, with the so-called “8:00am scramble” remaining a major source of frustration.
Older patients, those in work, and people with caring responsibilities are among those most affected.
The report also points to concerns about reduced continuity of care and shorter appointment times, contributing to declining public confidence in GP services.
Hospitals feeling the strain
The findings reinforce concerns raised earlier this week about pressure on emergency departments and delays in care.
By failing to invest sufficiently in primary and preventative services, the report suggests more patients are reaching crisis point — increasing demand for hospital treatment that could otherwise have been avoided.
Call for urgent action
The Committee is calling on the Welsh Government to shift more healthcare services into the community, backed by sustained investment and reform of the funding system.
Committee chair Peter Fox said: “General practice and primary care are the cornerstone of our NHS.
“If we are to ease the growing pressures across the whole health system, we must ensure people can access services closer to home and receive treatment earlier.”
Healthcare leaders, including the British Medical Association and the Royal College of General Practitioners, have also warned that without decisive action, GP services will continue to deteriorate.
The report concludes that unless primary care is strengthened, pressure on hospitals will continue to grow — leaving patients facing longer waits and reduced access to treatment.
-

 News6 days ago
News6 days agoWelsh Government outlines progress on flood resilience plans
-

 Community5 days ago
Community5 days agoHero female officer keeps job after sexual touching finding
-

 Education4 days ago
Education4 days agoYsgol Henry Tudor reassures parents over Sikh ceremonial kirpan
-

 Business5 days ago
Business5 days agoPopular Italian restaurant hit with £278,000 tax bill plus £186,000 fine
-

 Health6 days ago
Health6 days agoClash over Withybush Hospital services as Paul Davies challenges First Minister
-

 Crime6 days ago
Crime6 days agoHakin motorist banned after drink-drive crash
-

 Farming6 days ago
Farming6 days agoExperts warn Senedd of ‘systemic failure’ to enforce animal welfare laws in Wales
-

 Entertainment6 days ago
Entertainment6 days agoDuffy to tell her story in new Disney+ documentary