Health
Locked up for Autism: Thousands detained under mental health law

“He didn’t break the law. He just needed help. Now he’s locked in a hospital hundreds of miles away.” — Alun, father of a detained 19-year-old
IN SECURE hospitals across England and Wales, more than 2,000 people with autism or learning disabilities remain locked away under mental health laws — despite never committing a crime.
Many are detained under the Mental Health Act 1983, often after being taken by police during a mental health crisis. The vast majority have no mental illness diagnosis. Some are teenagers. A few have been there for decades.
“It’s a human rights scandal,” said Dan Scorer of Mencap. “They’re being institutionalised because society hasn’t built the support they need.”
Autism is not a mental illness. It is widely recognised that for most autistic people, care in an inpatient unit is rarely helpful – in fact, it can be deeply damaging.
The average length of stay is around 4.6 years.
The overwhelming majority (92%) of autistic people and people with a learning disability who are detained in hospitals are put there using the Mental Health Act of 1983.
A NEED FOR URGENT REFORM
For years, the National Autistic Society and tens of thousands of campaigners have called for changes to mental health law.
Reform has been promised, and a bill is making its way through Parliament. However, the government will not commit to funding the reforms the legislation will enact. Even then, campaigners say the law change will not end the scandal of detention.
In April, Denise Cavanagh from Hook, a founder of the Stolen Lives campaign, told BBC Wales that she believed people would still be detained via other laws, including the Mental Capacity Act.
She added: “People with learning disabilities often end up in hospitals because there’s a breakdown in housing and community care, and it’s the only place they can go.
“So, if that community care isn’t there, there is nowhere for them to go and they’ll still be detained.”
And even though health is devolved to Wales, the Welsh Government is relying on a Westminster bill to improve how people with learning disabilities and autism are supported during a crisis.
“THEY CAME WITH HANDCUFFS”
Michelle, from Wiltshire, recounts the day her autistic daughter was detained after a meltdown in a supermarket.
“She was 23. She was overwhelmed. She panicked. That’s all. But the police came and took her away. That was three years ago. She hasn’t been home since.”
Michelle’s story is one of many. Some families describe wards where patients are sedated, isolated, and cut off from loved ones.
Bethany – whose surname cannot be published – was locked in a hospital room in Northampton as a teenager. Her only access to the outside world was through a tiny hatch in the door.
Her father, Jeremy, said he could only see his daughter through a plastic screen or through the six-inch hatch.
“It was cruel. It was torture for my daughter,” he said.
“It broke her human rights, her right to family life, her right to freedom from degrading treatment.”
Even now, several years on from Jeremy’s interview on Radio Four regarding Bethany’s treatment, little has changed. In fact, the data shows a worrying trend towards increased detention of those with mental illness or specific learning difficulties.
NO WAY OUT
Official NHS data reveals the extent of the crisis:
Over 52,000 people were detained under the Mental Health Act in April 2024 — the highest figure in five years.
Over 2,000 of those are autistic or have a learning disability.
As of May 2025, 2,025 autistic people and people with a learning disability are in mental health hospitals in England. Of these, 1,455 (72%) are autistic.
There are 240 under-18s in inpatient units who are autistic or have a learning disability. Of these, 230 (96%) are autistic.
The number of autistic people without a learning disability detained in mental health hospitals has increased by 141% since 2015.
This is the most up-to-date record of how many autistic people and people with a learning disability are currently in mental health hospitals in England.
Despite some progress moving people with a learning disability out of hospitals and into the community, the number of autistic people detained has increased. In 2015, autistic people made up 38% of the total number in hospitals, now it is 72%.
Around 60% of learning disability or autism inpatients have no mental illness diagnosis.
Detained patients are often placed in “out-of-area” units, sometimes hundreds of miles from home.
Toni Dymond, an autistic woman, was detained for over 20 years in psychiatric care without a criminal charge.
“She was isolated, broken,” said her brother in a statement. “It wasn’t treatment. It was abandonment.”
34,685 people were detained by police under Section 136 of the Mental Health Act in 2022–23.
Over 60% were transported in police vehicles, not ambulances.
Autistic woman and author of the memoir Unbroken, Alexis Quinn, spent three years “locked inside” various mental health hospitals, including Assessment and Treatment Units (ATU).
She says: “I was detained under the Mental Health Act and remained so for most of my stay. The Mental Health Act is a piece of legislation which provides a legal framework to detain people when they are mentally ill and require treatment to get better. The interesting thing about a treatment order for an autistic person is that autism is not a mental health condition.
“Whilst mental illnesses, such as depression and anxiety, can be treated, for autistic people, this has to be done in a way that reflects their needs and understands autism.
“When I was detained under the Mental Health Act, I felt like this was because of behaviour relating to my autism, not because I was mentally ill; the whole process lacked any understanding of the difference between autism and mental illness.”
CHANGE PROMISED, BUT NO MONEY ON THE TABLE
The Mental Health Bill, which is currently going through Parliament, will stop people with a learning disability and autistic people from being detained for treatment. However, the government have said that this change to the law will not be enforced until there is sufficient community support. That means the law will not come into effect until there are enough resources to support its operation. There is no commitment to provide that funding.
The Challenging Behaviour Foundation, a national charity, wants a clear plan, co-produced with people with lived experience, families, and those working within the different parts of the system, setting out what steps will be taken to develop this support and accompanied by the resources to make it happen.
The National Autistic Society says: “We are calling on the government to urgently publish a comprehensive and fully-costed plan for how it intends to build this support.”
So far, that call has been met with silence.
Health
FOI raises fresh questions over plan to close Pontyates GP surgery

Health board accused of misleading claims over recruitment as pressure mounts ahead of final decision
A FREEDOM of Information disclosure has raised serious questions over plans to close Meddygfa’r Sarn in Pontyates, with claims the health board failed to properly attempt to recruit permanent doctors before recommending its shutdown.
The row centres on Hywel Dda University Health Board, which is due to make a final decision on the surgery’s future later this month.
An FOI response reveals that while the board cited a “lack of recruitment interest” in its January report, there is limited evidence of any recent, targeted recruitment campaign specifically aimed at the Pontyates practice.
Instead, the board confirmed that salaried GP roles were advertised in 2020 across its wider portfolio of managed practices — rather than as a focused effort to fill posts at Meddygfa’r Sarn itself. Those vacancies did not result in successful appointments.
‘No real attempt’
Independent Senedd candidate Carl Peters-Bond, who is also a patient at the surgery, has strongly criticised the health board, accusing it of presenting a misleading picture to justify closure.
He said: “They cited a lack of recruitment interest as justification for closing this surgery — but they never actually ran a proper recruitment campaign for it.
“Sending out general adverts years ago is not the same as making a serious, targeted effort to keep a vital community service alive.”
He also raised concerns about the consultation process, claiming it focused on the impact of closure rather than asking whether closure should happen at all.
Fully reliant on locums
The FOI confirms that Meddygfa’r Sarn currently has no salaried GPs and is entirely dependent on locum doctors.
While the health board says this model is unsustainable in the long term, the same disclosure shows several other managed practices across the region also rely heavily on locum staff — some to a significant degree.
Cost data included in the response suggests Meddygfa’r Sarn is not the most expensive practice per patient within the health board’s area.
Alternative options unclear
Another key issue raised by campaigners is the apparent lack of explored alternatives.
The FOI response indicates that the health board does not hold information on alternative local solutions, including potential relocation or different service models within the Pontyates area.
Campaigners argue this suggests closure was considered before all options had been properly examined.
A 52-page independent report submitted as part of the consultation process states that dispersing patients to other surgeries should only be considered as a last resort, after full recruitment efforts and capacity assessments have been carried out.
Health board position
Hywel Dda University Health Board maintains that the surgery, which serves around 4,350 patients, has faced long-standing recruitment difficulties and increasing reliance on temporary staff.
It says a Vacant Practice Panel concluded that dispersing patients to neighbouring surgeries would provide a more sustainable long-term solution.
The board has also acknowledged that transport and access concerns are likely to be a major issue for patients if the closure goes ahead, with a full Equality Impact Assessment expected to be considered before a final decision.
Decision later this month
The future of Meddygfa’r Sarn will be decided at a meeting of Hywel Dda University Health Board on Wednesday (May 28) at Yr Egin in Carmarthen.
With local anger growing and new questions emerging from the FOI disclosure, pressure is mounting on board members to reconsider the proposal.
Campaigners say the case now hinges on a simple question: whether enough was done to save the surgery before moving to close it.
Health
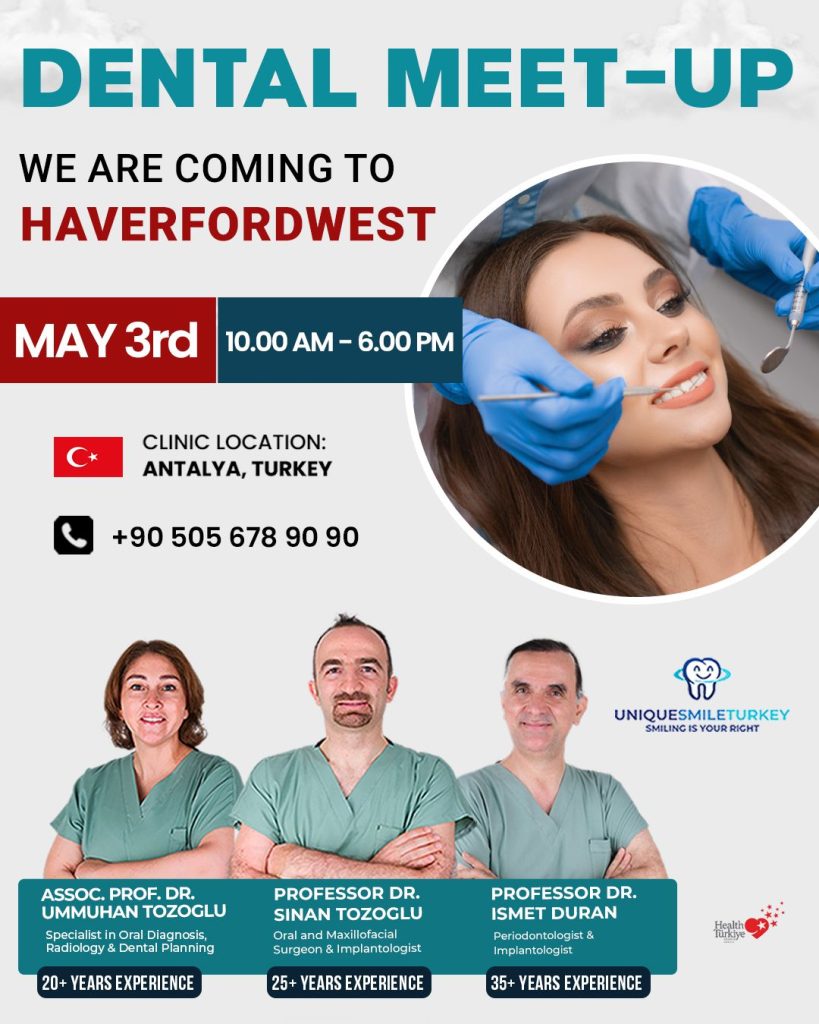
Turkish dental clinic to hold Haverfordwest meet-up
DENTISTS FROM ANTALYA TO VISIT COUNTY TOWN
A TURKISH dental clinic is running a dental meet-up in Haverfordwest this weekend as part of a promotional visit to Wales.
Unique Smile Turkey, which has a permanent office in Wales in Swansea, says its top dentists will be coming to Haverfordwest on Sunday (May 3).
The event is being advertised as a “Dental Meet-Up” and is scheduled to run from 10:00am to 6:00pm at the Mariners Hotel.
The visit features three clinicians: Assoc Prof Dr Ummuhan Tozoglu, described as a specialist in oral diagnosis, radiology and dental planning; Professor Dr Sinan Tozoglu, described as an oral and maxillofacial surgeon and implantologist; and Professor Dr Ismet Duran, described as a periodontologist and implantologist.
The team have between twenty and 35 years of experience in their respective fields.
A contact number has also been provided for enquiries: +90 505 678 90 90.
The visit comes amid continuing interest in dental tourism, with many people in the UK looking overseas for cosmetic dentistry, implants and other private dental treatment.
Turkey has become one of the most popular destinations for such treatment, although patients are generally urged to make careful checks before committing to any procedure abroad, including aftercare arrangements, qualifications, insurance, treatment plans and what support would be available if complications arise after returning home.
Health
Welsh public backs urgent action on dementia ahead of Senedd elections

Calls grow for diagnosis, care and support to become national priority
NEW figures reveal overwhelming public demand for dementia to be placed at the top of Wales’ political agenda, with voters urging action on diagnosis, treatment and support ahead of the Senedd elections.
Research by Alzheimer’s Society Cymru shows that 83% of people in Wales want dementia made a healthcare priority, while 69% believe it is currently overlooked and underfunded.
More than a thousand adults were surveyed, with the findings highlighting growing concern over diagnosis rates and access to care. Wales continues to record some of the lowest dementia diagnosis rates in the UK, leaving thousands of families without clarity or support.
Around 51,000 people are currently living with dementia in Wales, a figure expected to rise to 70,000 by 2040. Despite this, only 57% of people have received a formal diagnosis, with rates falling as low as 48% in rural areas such as Powys.
Improving diagnosis remains a key concern, with 91% of those surveyed saying access to timely diagnosis must improve, and 87% backing increased investment in diagnostic services. However, respondents also stressed that diagnosis alone is not enough, with 91% saying people with dementia must receive better support, including help for unpaid carers.
Ceri Parry, from Cardiff, said she was forced to retire early from her role as a headteacher at the age of 55 due to a lack of support for her mother, who was diagnosed with Alzheimer’s disease in 2020.
She said: “I fully support improving early and accurate diagnosis, but this must also come with improved support and care for families afterwards. There’s five years between my relatives’ diagnoses and nothing changed. On both occasions we left with a leaflet and the unknown.
“The wait for improved diagnosis, treatment and support needs to end. Dementia must be a top priority for the next Welsh Government, for families living with it now and for those who will face it in the future.
“We also found there was no diagnosis assessment available in the Welsh language. That’s a fundamental issue if a diagnosis is to be accurate and safe for people who speak Welsh as their first language. Ignoring someone’s identity is ignoring the person.”
The survey also found that visible action would be key to restoring public confidence, with 72% calling for improved dementia services, 64% backing more funding for research, and 63% wanting better access to treatments.
Gemma Roberts, National Influencing Manager at Alzheimer’s Society Cymru, said: “Dementia is Wales’s biggest killer and one of the greatest health and social care challenges we face.
“Hope is on the horizon with new treatments and faster, more accurate diagnosis, but the system is not keeping pace. Without urgent transformation, people in Wales risk missing out.
“We are at a turning point. The next Welsh Government must deliver a bold new dementia strategy that transforms diagnosis and ensures access to quality care, treatments and support.”
-

 News20 hours ago
News20 hours agoBaby in critical condition after Fishguard emergency
-

 Community6 days ago
Community6 days agoDogs removed after welfare concerns at Milford Haven property
-

 Crime7 days ago
Crime7 days agoPembrokeshire hairdresser avoids prison after pub assault
-

 Crime7 days ago
Crime7 days agoPembrokeshire man charged with making hundreds of indecent images of children
-

 Business7 days ago
Business7 days agoHandcrafted garden furniture built to last across Pembrokeshire
-

 Charity7 days ago
Charity7 days agoRow erupts at Spitfire museum after Reform poster displayed at charity premises
-

 Community7 days ago
Community7 days agoCancer patients targeted with parking fines outside Haverfordwest support centre
-

 Community2 days ago
Community2 days agoTenby phone signal crisis goes national as businesses warn of summer disruption