Health
Call for reform: Campaigners urge minister to record BSL complaints

CAMPAIGNERS in Wales are calling on the Welsh Government to amend NHS regulations to ensure complaints about British Sign Language (BSL) interpreter services are properly recorded, amid concerns that Deaf patients are being let down by the system.
The Cardiff Deaf Support Group has urged Senedd members to press Health Minister Jeremy Miles MS to change the ‘Putting Things Right’ (PTR) regulations. Currently, concerns about BSL interpreter services in NHS Wales hospitals and GP practices are not recorded as a separate category, making it difficult to assess the scale of issues.
Impact on patients in Pembrokeshire
While the campaign originates in Cardiff, the issue affects Deaf patients across Wales, including those using services at Withybush Hospital and GP surgeries in Pembrokeshire.
Cedric Moon, secretary of the Cardiff Deaf Support Group, requested data on BSL-related complaints under the Freedom of Information (FoI) Act. However, responses from Cardiff and Vale University Health Board (UHB) confirmed that such concerns are not centrally recorded and would require a manual search of records—an effort the UHB says exceeds the time and cost limits set under FoI laws.
Health boards, including Hywel Dda UHB, which oversees healthcare in Pembrokeshire, are required to publish annual reports on patient complaints. However, concerns about BSL interpretation failings are not reported separately, making it unclear how many Deaf patients have struggled to access NHS services in the county.
Appeal to the health minister
In his letter to Senedd member Rhys ab Owen, Mr Moon called for action to amend regulations so that BSL-related complaints are documented and made publicly available in NHS Wales annual reports.
Regulation 51 of the PTR framework states that health boards must produce an annual report detailing the nature and number of concerns received. However, without a specific category for BSL issues, these complaints are effectively invisible.
“We need accountability,” said Mr Moon. “BSL users in Wales should have the same rights as everyone else when it comes to raising concerns about NHS services.”
A systemic issue
The Cardiff and Vale UHB’s refusal to provide data highlights a wider problem across NHS Wales, campaigners argue. The exemption under Section 12 of the Freedom of Information Act—citing the excessive cost of retrieving data—has been used to deny access to statistics on multiple occasions.
Hywel Dda UHB has not yet confirmed whether similar issues exist locally, but Deaf patients in Pembrokeshire rely on interpreter services for GP and hospital appointments, and any gaps in provision could affect their ability to access care.
Mr Moon is now urging the health minister to intervene and update the regulations to ensure all health boards, including Hywel Dda, are required to record and report on BSL interpreter service complaints.
The Herald has contacted the Welsh Government and Hywel Dda UHB for a response.
Health
Decision pending on adult mental health referral pathway

HYWEL DDA University Health Board will decide next week whether to make changes to the GP referral pathway for routine adult mental health services permanent.
The decision will be taken at a public Board meeting on Thursday (Mar 26).
Board members will consider a proposal to formalise changes already introduced in Ceredigion and, if approved, roll out the revised pathway across Pembrokeshire and Carmarthenshire.
Since March 2025, adults in Ceredigion seeking routine mental health support have been advised by their GP to contact the NHS 111 Wales ‘Press 2’ service, rather than being referred directly to the county’s Community Mental Health Team.
The temporary change was introduced in response to ongoing staffing shortages. Health Board officials say the approach has helped maintain timely access to face-to-face assessments for those who need them, while directing initial contact through a single access point.
The 111 ‘Press 2’ service provides telephone assessments by local wellbeing practitioners, supervised by registered mental health nurses, offering advice, support and onward referrals where required.
At its November 2025 meeting, the Board agreed to extend the temporary pathway until the end of March 2026. A nine-week engagement exercise followed, running from December 8 to February 9, to gather feedback from patients, professionals and stakeholders on the potential long-term impact.
Andrew Carruthers, Chief Operating Officer at Hywel Dda University Health Board, said: “I would like to thank everyone who took the time to share their views and experiences.
“I would also like to thank West Wales Action for Mental Health for supporting engagement with patients, including those with lived experience, alongside GPs, primary care teams, mental health staff and third sector partners.
“Our priority is to ensure mental health services remain accessible, fair and sustainable. The temporary changes in Ceredigion have shown some positive benefits, and the feedback we have received from across the three counties will play an important role in shaping the Board’s decision.”
The Board will review all evidence and feedback before making a final decision on the future of the adult mental health referral pathway.
GPs will continue to refer patients with urgent or complex needs directly to community mental health teams where appropriate, and have access to a dedicated NHS 111 professional line for additional clinical advice.
Further details, including the full Board papers, are available here:
https://biphdd.gig.cymru/amdanom-ni/eich-bwrdd-iechyd/cyfarfodydd-y-bwrdd-2026/agenda-a-phapuraur-bwrdd-26-mawrth-2026/
The meeting will be streamed live from 9:30am on Thursday (Mar 26) via:
www.youtube.com/hywelddahealthboard1
Health
Parents urged to check children’s vaccinations after meningitis cases
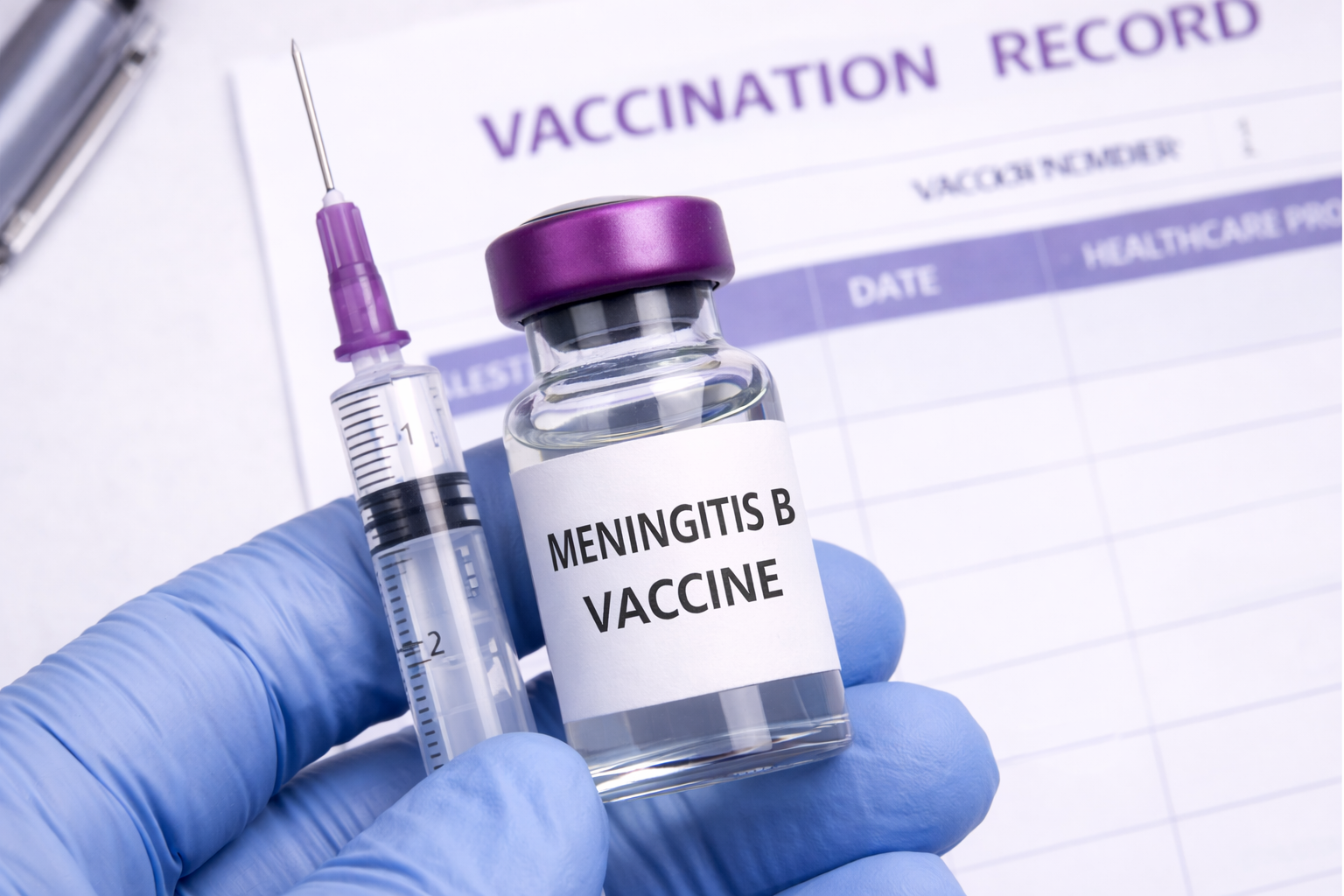
Local pharmacy reports MenB vaccine shortage amid rising concern
PARENTS and carers across west Wales are being urged to check their children’s vaccination status following recent meningitis cases in the UK.
The warning comes as a local pharmacy has confirmed a shortage of the Meningitis B (MenB) vaccine, highlighting growing pressure on supplies.
Mendus Pharmacy said it currently has no availability of the vaccine due to what it described as a nationwide supply issue.

In a statement, the pharmacy said: “We would like to inform our patients that, due to ongoing supply issues, we currently have no availability of the Meningitis B vaccine.
“Unfortunately, this is a nationwide shortage and all stock is currently unavailable.
“We understand this may be particularly concerning given the recent outbreak reported in Kent, and we completely appreciate the importance of timely vaccination.”
The pharmacy confirmed it is operating a waiting list and will contact patients once supplies return.
Health officials say keeping vaccinations up to date remains one of the most effective ways to prevent serious illness and reduce pressure on NHS services.
Dr Ardiana Gjini, Executive Director of Public Health at Hywel Dda University Health Board, urged parents to act.
She said: “Vaccination is one of the most effective ways we can protect children and young people from serious illness.
“Ensuring your child is fully vaccinated not only safeguards their health but also helps prevent the spread of infections within our communities.
“I strongly encourage all parents and carers to check their child’s vaccination status. If you are concerned that your child may have missed routine vaccinations, please speak to your GP.”
Meningococcal disease is a serious and potentially life-threatening infection that can lead to meningitis or septicaemia. While many people recover, some are left with long-term physical, neurological or psychological complications. Around one in ten cases can be fatal.
Although the disease can affect anyone, babies, young children, teenagers and young adults are at greatest risk.
In Wales, vaccines protecting against meningococcal strains A, B, C, W and Y are offered as part of the NHS immunisation programme. Infants receive the MenB vaccine, while teenagers are offered the MenACWY vaccine.
Latest figures from the Health Board show that uptake among 16-year-olds for the MenACWY vaccine stands at 76.4%, meaning a significant number of young people remain unprotected as they approach adulthood.
For younger children, uptake of the MenB vaccine is higher but still below the recommended 95% target. Around 92.8% of infants are vaccinated by their first birthday, rising slightly to 91.8% by their second.
Health officials say these figures reflect strong engagement from families and primary care teams but stress that continued vigilance is needed.
Families are being advised to check their child’s vaccination record with their GP or by contacting the Health Board directly. Parents should also ensure babies receive their scheduled MenB doses and that teenagers receive their MenACWY and 3-in-1 booster vaccines, which are currently being delivered in schools.
Parents are also urged to remain alert to the symptoms of meningitis and septicaemia and to seek urgent medical advice if they have concerns.
Further information on symptoms is available via NHS 111 Wales.
Health
NHS ‘on brink of collapse’ during Covid as inquiry exposes failures

Wales warned to act fast as damning report reveals staff trauma, delayed care and deadly gaps
THE UK’s healthcare system came perilously close to collapse during the Covid-19 pandemic, a major public inquiry has found, with Wales now facing pressure to act on urgent recommendations.
A landmark report published on Thursday (Mar 19) lays bare the scale of the crisis, concluding that hospitals across the UK – including in Wales – were pushed to “intolerable strain”, with some patients receiving lower levels of care and others left untreated altogether.
The findings come as First Minister Eluned Morgan welcomed the report and confirmed the Welsh Government will respond within six months.
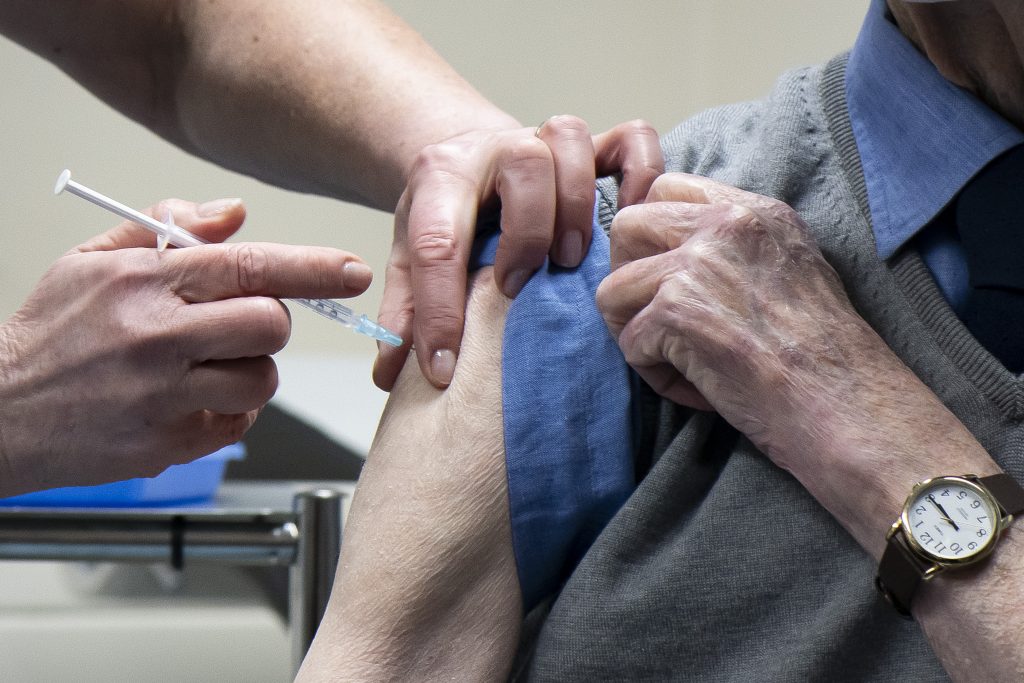
System “ill-prepared” for pandemic
The inquiry found the UK entered the pandemic in a weakened state, with staff shortages, too few hospital beds, and ageing infrastructure already placing pressure on services.
Healthcare systems “coped, but only just,” the report states, warning that collapse was only avoided due to the “almost superhuman efforts” of NHS staff.
Many workers suffered severe mental health impacts, with burnout and post-traumatic stress widespread across the workforce.
Patients died alone
Among the most distressing findings was the impact of strict hospital visiting rules.
Thousands of patients died without family by their side, while relatives were often forced to say goodbye over the phone or by text.
The report highlights how restrictions, though intended to save lives, caused lasting trauma for families across Wales and the UK.
Missed treatment and cancer delays
The inquiry also exposes the devastating knock-on effect on non-Covid care.
Planned operations were cancelled, screening programmes paused, and patients avoided hospitals out of fear – leading to delayed diagnoses and, in some cases, avoidable deaths.
Cancer treatment performance worsened, with late diagnoses contributing to increased mortality.
“Fundamental flaws” in response
Investigators identified serious failings in how the pandemic was handled, including:
- Early guidance that underestimated airborne transmission
- Shortages of PPE, leaving staff exposed
- Poor communication with vulnerable patients
- Inadequate planning for emergency and critical care capacity
These issues, the report says, put both patients and staff at greater risk.

NHS 111 and ambulances overwhelmed
Emergency systems also struggled to cope.
Demand for NHS 111 surged beyond capacity, while ambulance delays increased – even for life-threatening calls.
The report warns future pandemics could see similar failures unless urgent reforms are made.
Long Covid and hidden impact
The long-term effects of Covid are still being felt, with inconsistent care for Long Covid patients and ongoing uncertainty around treatment.
Meanwhile, millions of people who needed routine care remain affected by the backlog created during the pandemic.

Welsh Government response
First Minister Eluned Morgan said the Welsh Government would respond “openly and constructively” to the findings.
She acknowledged the significant impact on patients, staff and families and confirmed Wales will address the inquiry’s recommendations within the required six-month timeframe.
Urgent warnings for the future
The inquiry makes ten key recommendations, including:
- Expanding hospital and emergency capacity
- Improving infection control guidance
- Strengthening support for healthcare workers
- Better data systems to identify vulnerable patients
It warns that without action, the NHS may not withstand the next pandemic.
“We may not be so lucky next time”
In one of the report’s starkest conclusions, Baroness Hallett warned that healthcare systems came dangerously close to failure.
If the crisis had lasted longer – or hit harder – the NHS could have collapsed entirely.
The message is clear: Wales and the UK must prepare now, or risk repeating the same mistakes.
-

 Health7 days ago
Health7 days agoWelsh Ambulance Service to host bi-monthly Board meeting
-

 News6 days ago
News6 days agoRayner and Lammy visit Wales to discuss justice and community safety
-

 News5 days ago
News5 days agoFishguard linked to allegations in Many Tears Animal Rescue investigation
-

 News3 days ago
News3 days agoEmergency services flood Haverfordwest after reports of person in river
-

 Local Government6 days ago
Local Government6 days agoInvestigation confirmed after inspectors visit Many Tears Animal Rescue
-

 Business7 days ago
Business7 days agoWork set to begin on £50m hydrogen plant in Milford Haven
-

 Community7 days ago
Community7 days agoLocal charity hosts cancer awareness event in Cardigan
-

 Community7 days ago
Community7 days agoExtra £1m announced to help feed families across Wales































