Health
Leading pharmacies demand tougher regulation on online sale of weight-loss jabs

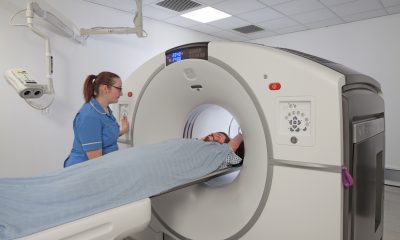
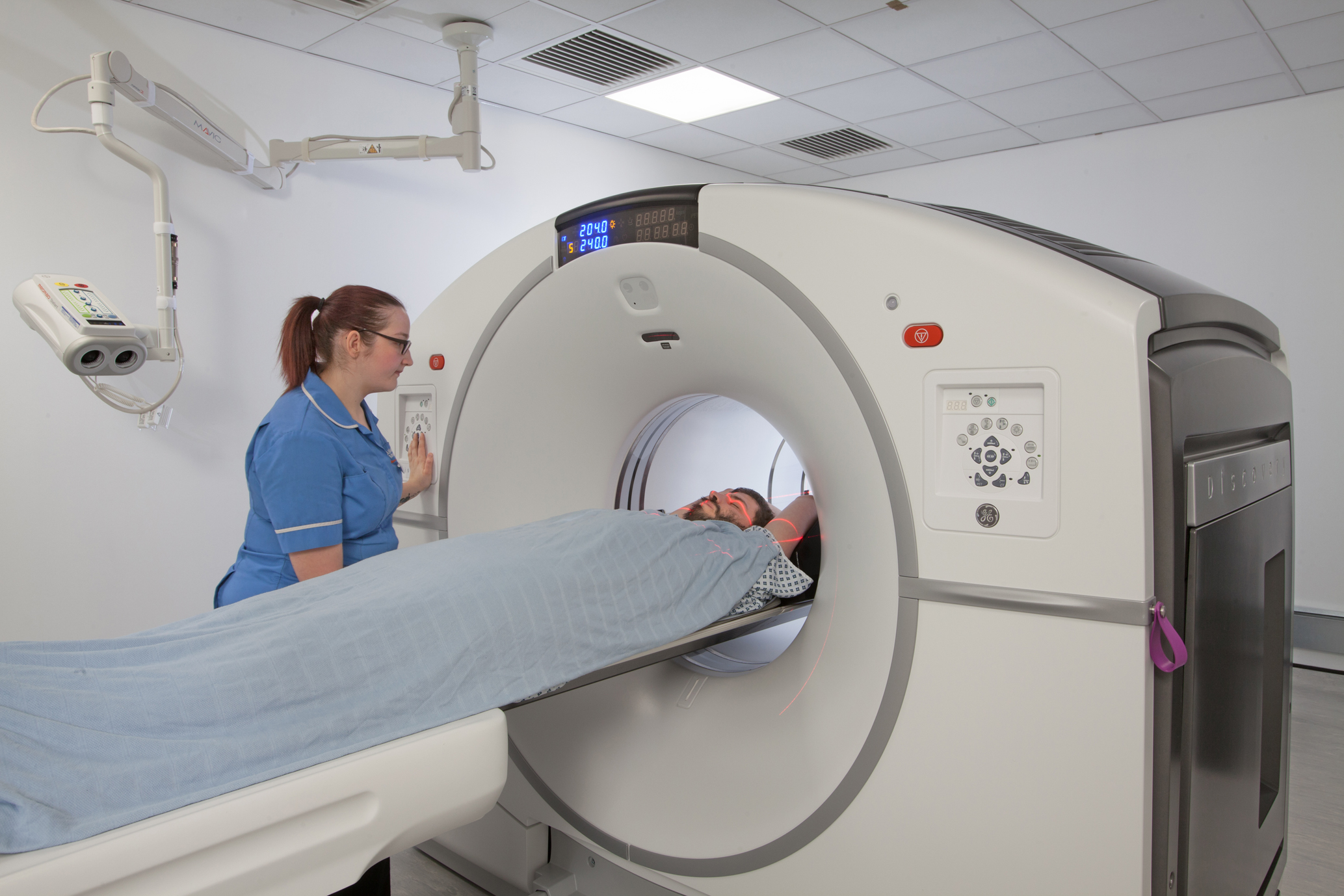
PHARMACIES are calling for stricter regulation of online sales of weight-loss injections, warning of risks to patient safety amid predictions of a surge in demand this year.
The National Pharmacy Association (NPA), representing independent community pharmacies, has urged the General Pharmaceutical Council (GPhC) to require more thorough consultations with patients before dispensing weight-loss injections and other high-risk medications online.
The NPA cautioned that existing regulations allow medicines to be supplied without adequate consultation or access to patient records, leaving patients vulnerable. They called for a mandatory two-way consultation process to ensure prescribers have a full understanding of patients’ medical histories before issuing such treatments.
Greater safeguards needed
Responding to draft GPhC guidelines, the NPA criticised the proposed safeguards, stating they “still leave the door open for medicines to be prescribed and supplied without appropriate two-way patient consultation or access to a full clinical picture, particularly with high-risk medicines.”
The association recommended prescribers engage in direct dialogue with patients—either in person or via telephone—before offering weight-loss medications such as Mounjaro injections. The NPA also stressed the importance of obtaining comprehensive medical histories, rather than relying solely on online questionnaires.
Nick Kaye, Chair of the National Pharmacy Association, said:
“Obesity is one of the biggest challenges facing our country, and pharmacies want to play their part in helping patients achieve and maintain a healthy weight.
“Weight-loss injections can be effective when prescribed as part of a carefully managed programme, but the current regulations allow some patients to access these medications inappropriately, without proper consultation or examination of medical records.”
Addressing rising demand
The call for tighter regulations comes as demand for weight-loss treatments is expected to rise, with the government planning to expand the rollout of such medications. Many pharmacies already dispense weight-loss treatments or include them in private weight-loss programmes, emphasising a need for best practices to prioritise patient safety.
The NPA highlighted cases of patients who had been inappropriately prescribed weight-loss injections, including individuals with eating disorders or those with body mass indexes (BMI) outside the licensed range. Such cases increase the risk of severe adverse effects.
Kaye added:
“Medicines are not like ordinary goods for sale; they must be handled with great care because they have the power to harm as well as to heal. We urge the GPhC to make a full consultation compulsory for high-risk medicines and ensure supply is prioritised for those with the greatest clinical need, including those with type 2 diabetes.”
Warning against unregulated sellers
The NPA and the Medicines and Healthcare products Regulatory Agency (MHRA) have also warned against purchasing weight-loss injections from unregulated sources, such as beauty salons or social media platforms. Counterfeit medications from these suppliers pose significant health risks.
The NPA advised patients to consult a pharmacist if they are unsure about weight-loss treatments, ensuring they receive safe and effective care as part of a programme to achieve sustainable lifestyle changes.
Health
New NHS regional body raises questions over future hospital services in Pembrokeshire
Health bosses promise better joined-up care — but patients will want assurances over Withybush and travel distances
PEMBROKESHIRE patients are likely to be asking what a major NHS shake-up means for the future of hospital services closer to home after a new regional health body formally took over planning across south west Wales.
Health chiefs this week confirmed that regional working has formally transferred from ARCH (A Regional Collaboration for Health) to the South West Wales Regional Joint Committee (RJC), bringing together Hywel Dda and Swansea Bay university health boards under a new leadership structure.
The move is being presented by NHS leaders as a way to improve coordination, reduce waiting times and strengthen specialist healthcare across the region.
Key programmes expected to continue under the new body include cancer care, stroke services, vascular treatment, orthopaedics, pathology and eye care.
But for many in Pembrokeshire, the announcement may trigger familiar concerns about whether “regional working” could eventually mean more services being delivered further east, requiring patients to travel longer distances to Carmarthen or Swansea.
Withybush Hospital remains fiercely valued by local communities, and previous changes to hospital services have often sparked strong public reaction.
For patients in more rural parts of Pembrokeshire — including St Davids, Fishguard, Newport, Crymych and Tenby — access to healthcare can already involve journeys of 40 to 60 miles or more for appointments and treatment.
While health officials insist the new structure is about improving care and making better use of expertise across the region, questions are likely to be asked locally over how Pembrokeshire’s voice will be represented in decisions affecting frontline services.
Among the issues patients may want clarified are whether services currently provided at Withybush could be affected, how travel difficulties for rural communities will be considered, and whether the new regional approach will improve care locally or lead to greater centralisation.
The Regional Joint Committee replaces ARCH, which since 2015 brought together Swansea Bay University Health Board, Hywel Dda University Health Board and Swansea University to support healthcare innovation and service planning.
Health leaders say the new committee will continue to support research, technology and partnership working, while involving patients and communities in shaping services.
But in here Pembrokeshire, many will this plan weaken Withybush, not strengthen it.
Business
Why mental health support is now critical for Welsh businesses

MENTAL HEALTH support has become a key issue for businesses in Wales as employers face growing pressure to help staff manage financial strain, stress and wellbeing at work.
The issue is being highlighted during Mental Health Awareness Week, with new insight from Reed showing that support for employee wellbeing is now an important part of attracting and retaining staff.
Workers in Wales said they need an annual income of £42,000 to live comfortably, compared with an average regional salary of £36,000. That leaves a “comfort gap” of £6,000.
Reed’s latest salary guides also show that 71% of workers say pay has become more important since the cost-of-living crisis, with many employees feeling the pressure of rising everyday costs.
The strain is not only financial. Separate research shows almost one in four workers in Wales, 24%, say they have previously been formally diagnosed with a mental health condition — the highest reported proportion of any UK region.
Pay alone ‘not enough’
Becky Hole, Regional Director at Reed, said employers now needed to look beyond salary alone.
She said: “In Wales, financial pressure and mental health challenges are closely linked. Our data shows that many employees are placing greater importance on stability and support, particularly where salary growth is constrained.
“This means benefits that support work-life balance and mental wellbeing are becoming a much more important part of how valued people feel at work.
“Organisations that prioritise employee wellbeing also benefit in tangible ways. By providing stronger support for mental health, employers can lower staff turnover and reduce the long-term costs linked to ongoing recruitment and the loss of skilled, experienced employees.”
What workers want
WHEN asked what would help them manage stress, 35% of workers in Wales said they wanted more flexible working, 34% wanted better mental health training for managers, and 30% wanted clearer communication about support already available.
However, Reed said there remains a gap between what workers want and what they receive.
The most common benefits currently reported by workers in Wales are onsite parking, at 28%, flexi time, at 26%, and hybrid working, at 23%. Nearly one in five workers, 18%, said they receive no benefits at all.
Ms Hole added: “What this shows is a disconnect between what employees say would most help them manage stress and how clearly mental health support is currently embedded and communicated.
“However, Wales stands out when it comes to flexi time, with a higher proportion of employers offering this benefit compared to other regions — a positive step given its proven role in supporting employee wellbeing and work-life balance.
“Flexible working, open conversations about mental health and managers who are properly trained all come through strongly as priorities.
“Employers have a responsibility to look after their people, and those who want to help their workforce truly destress need to ensure their benefits are visible, accessible and actively support everyday mental resilience.”
Reed said businesses that take wellbeing seriously are more likely to retain skills, stability and trust over the long term.
Health
Welsh adults using harmful habits to manage mental health

NEW POLLING shows more than two-thirds of adults in Wales are using potentially harmful coping mechanisms when feeling stressed, anxious or low.
The Mental Health Foundation said the findings, released for Mental Health Awareness Week, show a need for the new Welsh Government to prioritise prevention and action on poor mental health.
The survey found that 69% of adults in Wales had taken harmful actions to cope with their mental health in the past month.
More than a third, 36%, said they had spent time isolating themselves from others, while 34% reported spending more time scrolling social media or going online as a way to deal with anxiety, stress or low mood.
Other commonly reported behaviours included comfort eating or overeating, at 27%, and oversleeping or not getting out of bed, at 31%.
The Mental Health Foundation said these behaviours were concerning because evidence suggests they can make mental health worse over time.
However, the polling also found that many people in Wales are taking positive steps to support their wellbeing.
More than four in five adults, 84%, had taken at least one helpful action to support their mental health. The most common were accessing nature, at 41%, doing something enjoyable such as a hobby, at 37%, and taking part in physical activity or prioritising sleep and rest, at 35%.
The poll of 1,015 people in Wales was carried out by Opinium on behalf of the Mental Health Foundation. It was released to mark Mental Health Awareness Week, which runs from May 11 to 17.
Catherine Razzell, Policy and Public Affairs Manager at the Mental Health Foundation, said: “This polling tells us that, here in Wales, there is a concerning degree of harmful actions taken by people as a way of dealing with their feelings of poor mental health, such as doomscrolling or overeating.
“We are hopeful to see positive actions being taken by individuals to help maintain and improve good mental health. Tried and trusted activities such as connecting with nature, which many of us are fortunate to have access to in Wales, and taking part in physical exercise and rest, in equal measure, are all known to support our mental health.”
Calls for action
The polling found that nearly two-thirds of people in Wales, 64%, are using at least one harmful coping mechanism alongside positive actions.
Only one in five, 20%, reported taking only helpful actions to support their mental health.
The Mental Health Foundation said the results come at a significant moment following the Senedd election, with a new Welsh Government now in place.
Ms Razzell added: “Whilst it is good news people are finding ways to prioritise and protect their mental health and support those around them, more action is needed from our governments to create the conditions to support good mental health.
“We are seeing a once in a generation change politically in Wales. We are one year into the new ten-year mental health strategy for Wales and are keen to see how the new government will implement and resource this.
“In addition to a resourced focus on prevention, which we know has long-term economic benefits, we know that inequalities exist here that are huge barriers to good mental health, keeping people locked in poverty for generations.
“We want to see these issues tackled head-on by the new government for Wales. Now is the time for action and not talk.”
Mental Health Awareness Week is run by the Mental Health Foundation. This year’s theme is “Action”.
-

 News2 days ago
News2 days agoPalestine pledge backed by 36 new Senedd Members
-

 Crime4 days ago
Crime4 days agoTeenager banned from roads after being caught six times over drug-drive limit
-

 Crime4 days ago
Crime4 days agoMan threatens to torch Silverdale Lodge through ‘demon drink’, court hears
-

 Crime4 days ago
Crime4 days agoMan sentenced for stalking women and threatening to torch home
-

 Crime4 days ago
Crime4 days agoViolent man jailed after ‘Banksy’ claims and campaign of domestic abuse
-

 Community13 hours ago
Community13 hours agoSurfers take sewage protest to Broad Haven beach
-

 Community6 days ago
Community6 days agoConcern grows after child hospitalised following Tenby sea swim
-

 Local Government6 days ago
Local Government6 days agoCouncil leadership hopeful responds after anti-Tory rally photos surface