Health
NHS ‘on brink of collapse’ during Covid as inquiry exposes failures

Wales warned to act fast as damning report reveals staff trauma, delayed care and deadly gaps
THE UK’s healthcare system came perilously close to collapse during the Covid-19 pandemic, a major public inquiry has found, with Wales now facing pressure to act on urgent recommendations.
A landmark report published on Thursday (Mar 19) lays bare the scale of the crisis, concluding that hospitals across the UK – including in Wales – were pushed to “intolerable strain”, with some patients receiving lower levels of care and others left untreated altogether.
The findings come as First Minister Eluned Morgan welcomed the report and confirmed the Welsh Government will respond within six months.
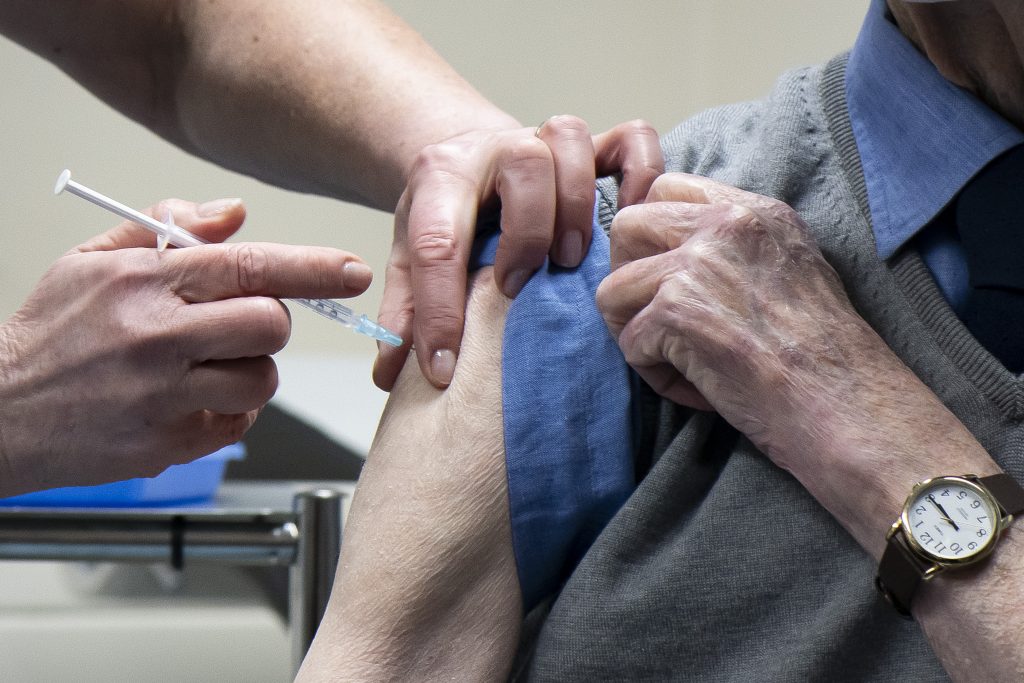
System “ill-prepared” for pandemic
The inquiry found the UK entered the pandemic in a weakened state, with staff shortages, too few hospital beds, and ageing infrastructure already placing pressure on services.
Healthcare systems “coped, but only just,” the report states, warning that collapse was only avoided due to the “almost superhuman efforts” of NHS staff.
Many workers suffered severe mental health impacts, with burnout and post-traumatic stress widespread across the workforce.
Patients died alone
Among the most distressing findings was the impact of strict hospital visiting rules.
Thousands of patients died without family by their side, while relatives were often forced to say goodbye over the phone or by text.
The report highlights how restrictions, though intended to save lives, caused lasting trauma for families across Wales and the UK.
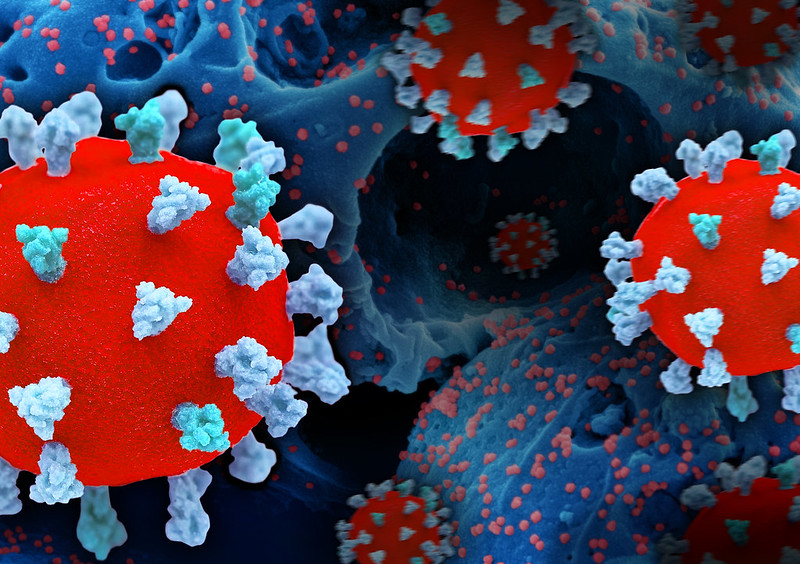
Missed treatment and cancer delays
The inquiry also exposes the devastating knock-on effect on non-Covid care.
Planned operations were cancelled, screening programmes paused, and patients avoided hospitals out of fear – leading to delayed diagnoses and, in some cases, avoidable deaths.
Cancer treatment performance worsened, with late diagnoses contributing to increased mortality.
“Fundamental flaws” in response
Investigators identified serious failings in how the pandemic was handled, including:
- Early guidance that underestimated airborne transmission
- Shortages of PPE, leaving staff exposed
- Poor communication with vulnerable patients
- Inadequate planning for emergency and critical care capacity
These issues, the report says, put both patients and staff at greater risk.

NHS 111 and ambulances overwhelmed
Emergency systems also struggled to cope.
Demand for NHS 111 surged beyond capacity, while ambulance delays increased – even for life-threatening calls.
The report warns future pandemics could see similar failures unless urgent reforms are made.
Long Covid and hidden impact
The long-term effects of Covid are still being felt, with inconsistent care for Long Covid patients and ongoing uncertainty around treatment.
Meanwhile, millions of people who needed routine care remain affected by the backlog created during the pandemic.

Welsh Government response
First Minister Eluned Morgan said the Welsh Government would respond “openly and constructively” to the findings.
She acknowledged the significant impact on patients, staff and families and confirmed Wales will address the inquiry’s recommendations within the required six-month timeframe.
Urgent warnings for the future
The inquiry makes ten key recommendations, including:
- Expanding hospital and emergency capacity
- Improving infection control guidance
- Strengthening support for healthcare workers
- Better data systems to identify vulnerable patients
It warns that without action, the NHS may not withstand the next pandemic.
“We may not be so lucky next time”
In one of the report’s starkest conclusions, Baroness Hallett warned that healthcare systems came dangerously close to failure.
If the crisis had lasted longer – or hit harder – the NHS could have collapsed entirely.
The message is clear: Wales and the UK must prepare now, or risk repeating the same mistakes.
Health
NHS waiting list falls — but cancer delays and diagnostic backlog worsen

Record progress claimed by Welsh Government as critics warn key targets are still being missed
THE NHS in Wales has recorded its biggest-ever monthly drop in waiting lists, according to new figures released on Thursday (Mar 19), but worsening cancer treatment times and a growing diagnostic backlog highlight ongoing pressure on services.
The latest data shows the waiting list fell by 27,900 in January — the largest monthly reduction on record — marking eight consecutive months of decline.
Average waiting times have now dropped to around 18 weeks, the lowest level since before the pandemic.

Cancer target slips further
Despite the overall progress, performance in cancer care has deteriorated.
Just 57% of patients began treatment within the 62-day target in January — down from 60.7% in December and well below the 75% target.
Diagnostic delays at highest level in two years

The figures also show growing pressure in diagnostic services.
Around 135,300 patient pathways were waiting for diagnostic tests in January, with more than 48,300 waiting longer than the eight-week target — the highest level recorded since January 2024.
These delays can have a knock-on effect on treatment, as patients often cannot begin care until tests and scans are completed.
Emergency care targets still missed
Performance in emergency departments remains well below national targets.
Only 63.7% of patients spent less than four hours in A&E, against a target of 95%.
Nearly 10,000 patients (9,817) waited more than 12 hours in January, despite a target of zero.
Ambulance response times for life-threatening “red” calls averaged 8 minutes 54 seconds.
However, separate February data shows some improvement, with faster response times and reduced handover delays at hospitals.

Long waits remain far higher than England
While long waits have reduced overall, they remain significantly higher than in England.
More than 5,200 patients in Wales are still waiting over two years for treatment, compared with around 200 in England.
The Welsh Government had previously pledged to eliminate these waits by March 2023 and again by March 2024.
West Wales focus: Hywel Dda sees progress — but pressure remains
In west Wales, Hywel Dda University Health Board is increasing activity to tackle waiting times, supported by additional Welsh Government funding.
Health Secretary Jeremy Miles is visiting Prince Philip Hospital in Llanelli as part of efforts to highlight improvements, including increased outpatient appointments and record levels of operations.
Across Wales, health boards have delivered an additional 187,000 outpatient appointments and 37,000 cataract operations.
However, hospitals serving Pembrokeshire, Carmarthenshire and Ceredigion continue to face sustained demand.
Emergency departments across the Hywel Dda area have been operating under “extreme pressure” in recent months, with winter demand, staffing challenges and delays in patient discharge continuing to impact performance.
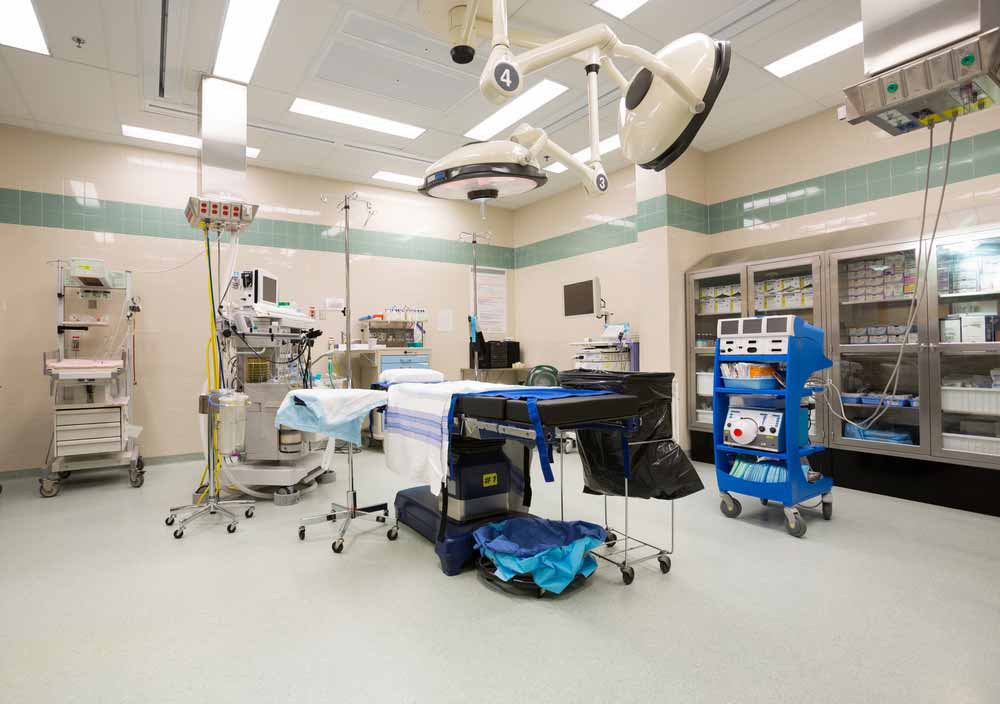
Political row over NHS performance
Welsh Government ministers say the figures show “real, tangible progress” in reducing waiting times.
Health Secretary Jeremy Miles said: “The waiting list has fallen for the eighth month in a row, a new record reduction, and the longest waits are down yet again.”
However, opposition parties say the improvements are not being felt where it matters most.
Peter Fox MS, Chair of the Senedd’s Health and Social Care Committee, said: “Cancer waiting times are worsening, with fewer patients starting treatment on time and no sign of sustained improvement.”
Reform UK Senedd Member James Evans MS added: “The waiting list for diagnosis is the highest we’ve seen for over two years, with no credible plan to fix the NHS.”
Welsh NHS Confederation
Responding to the NHS Wales activity and performance statistics for December and January, director of the Welsh NHS Confederation, Darren Hughes, said: “It’s encouraging to see continued month-on-month improvements in NHS waiting times, now for the eighth consecutive month. We commend the hard work of NHS staff and leaders who are driving this noteworthy progress.

“However, urgent and emergency care pressures remain. So, while targeted funding to boost progress in scheduled care is welcome, to achieve sustainable, long-term improvements across the breadth of health and social care, we need a more robust, whole-system approach that tackles the root causes of challenges.
“So far, what we’ve seen in party manifestos do not go anywhere near far enough to deliver the transformation needed to ensure the sustainability of our health and care services so they deliver for the people of Wales. It is not simply about having more beds, more diagnostic centres or more surgical hubs, we need a long-term commitment to deliver for the people of Wales.
“We need a long-term capital investment strategy to modernise NHS estates and infrastructure (including digital), an achievable plan to stabilise social care, an all-Wales long-term workforce plan for the NHS and social care workforce, joint performance and financial frameworks, and a cross-governmental shift towards prevention to drive down demand on health and care services.”
“It’s not easy but we need bravery and longer-term commitments from political parties – in line with the Well-being of Future Generations Act – so the people of Wales can live healthier, longer lives.”
Mixed picture across Wales
The latest figures present a mixed picture.
While waiting lists are falling and average waits are improving, performance in cancer care, diagnostics and emergency services continues to lag behind targets.
For patients across west Wales, the data reflects both progress and ongoing pressure as the NHS continues to recover while demand for services remains high.
Health
Pioneering cancer hair loss support service funded for a further two years

HYWEL DDA Health Charities, the official charity of Hywel Dda University Health Board, is proud to announce a funding award to support Phase 2 of the Heads Up initiative, a unique service that provides expert, person-centred, holistic hair loss care for people affected by cancer treatment.
This funding will enable the continuation of the Heads Up service until 31 December 2027, following its successful launch in January 2024. The funding has been generously match-funded by two partner organisations: the Withybush Hospital Cancer Day Unit Appeal and Cancer Hair Care.
Hywel Dda University Health Board is the first Health Board in Wales to provide a comprehensive support service for chemotherapy-related hair loss. The service, which is delivered by Cancer Hair Care, connects healthcare professionals and haircare experts from local communities to empower patients to manage their hair loss journey with independence, dignity and choice.
Gina Beard, Lead Cancer Nurse, said: “We are incredibly grateful to our local communities for their generous donations, which have made this funding possible. Hair loss can be one of the most distressing side effects of cancer treatment, and this service helps patients feel heard, supported and equipped with practical tools and advice. Thanks to this funding, we can continue to offer inclusive, compassionate care that makes a real difference to people’s lives.”
The Heads Up initiative has already delivered thousands of touchpoints with patients, healthcare professionals and hairdressers across the Hywel Dda area. It offers tailored support for every stage of the hair loss journey, including headwear options, brow and lash care, and guidance on new hair growth. The service also provides training for nurses and local hairdressers, helping to build a community of informed professionals who can offer evidence-based support.
Nicola Llewelyn, Head of Hywel Dda Health Charities, said: “We are so thankful to everyone who has donated to Hywel Dda Health Charities. Your support enables us to fund projects like Heads Up that go beyond standard NHS provision and truly enhance patient care.”
Trish George, Treasurer of Withybush Hospital Cancer Day Unit Appeal, said: “Having funded the original pilot and Phase 1 of the Heads Up project in Pembrokeshire and witnessed its success, we are delighted to be able to fund the costs of delivering this exciting and beneficial project to many more Pembrokeshire residents over the next two years.”
Founder of Cancer Hair Care Jasmin Julia Gupta said: “So many of the service users have sent such heartfelt messages of thanks for the creative, compassionate and expert services they have received. We are delighted and privileged to continue this much needed service. It’s really a team effort and I would like to take this opportunity to thank all the patients, nursing and healthcare staff, funders and the dedicated hairdressers, who have supported this project in hospitals and within the community.
“We are looking for more hairdressers to join the project and would like to encourage hairdressers to contact Cancer Hair Care directly to show their interest via our website at www.cancerhaircare.co.uk or via email at [email protected].”
For more information about Hywel Dda Health Charities and how to support projects like Heads Up, please visit: https://hywelddahealthcharities.nhs.wales/
Pictured: NHS staff receive training in supporting patients with hair loss
Health
We need earlier diagnosis and better aftercare, says Maxine Hughes in new documentary

A NEW documentary will shine a spotlight on Wales’s cancer system, with journalist Maxine Hughes exploring the experiences of patients and the challenges they face from diagnosis to recovery.
Maxine Hughes: Canser ar ba gost? (Maxine Hughes: Cancer at what cost?) will air on S4C on Tuesday (Mar 17) at 9:00pm, and will also be available on S4C Clic and BBC iPlayer with Welsh and English subtitles.
In the programme, Hughes examines the reality of cancer care in Wales, raising concerns about delays in diagnosis and gaps in aftercare.
“The figures in Wales show that the situation is worse than ever,” she says. “Cancer can progress from one stage to another in a matter of months. That can be the difference between fighting the disease and dying.”
Hughes, now aged 45, discovered a lump in her breast while living in Washington DC. With access to private healthcare, she received a diagnosis of triple negative breast cancer and began chemotherapy within two weeks.
“People in Wales are shocked when I tell them how quickly treatment started,” she says. “I was diagnosed and within a fortnight I was already having my first chemotherapy session.”
The programme also features voices from across Wales, including Lowri Griffiths of Tenovus, who speaks about losing her friend Claire O’Shea after difficulties in securing a diagnosis. The charity now backs Claire’s Campaign, calling for cultural change in how women’s concerns are treated in healthcare settings.
“We want doctors and clinicians to listen to women,” Griffiths says. “If they say something is wrong with their body, they know best. We also need a new cancer strategy in Wales to cope with the rising number of cases.”
Dawn Larson, from Caernarfon, describes her own experience, praising the treatment she received but highlighting the lack of follow-up care.
“The team I had was amazing; they fixed me,” she says. “But then there was nothing.”
Larson explained that while routine screening is offered every three years for women over fifty, those who have undergone treatment typically receive annual checks, which she believes is not enough.
Hughes contrasts this with her own aftercare in the United States, where she receives scans and blood tests every six months for five years.
The documentary also highlights the work of Ffion Haf Hughes, founder of Judith’s Trust, which supports women recovering from serious illness with cosmetic and therapeutic treatments.
“A lot of women come to us with significant physical changes following surgery,” she says. “But there are specialists doing incredible work, and it shows that outcomes can be better.”
Viewers will see Ffion creating a temporary nipple and areola for Hughes, illustrating the role of post-treatment care in restoring confidence and wellbeing.
Reflecting on her own journey, Hughes says: “After surgery, I asked what I should do next, and I was told to go out and live my life. That stays with me. You have to keep going.”
Blending personal testimony with wider analysis, the programme seeks answers from decision-makers while highlighting the urgent need for improvements in cancer care across Wales.
-

 Health6 days ago
Health6 days agoWelsh Ambulance Service to host bi-monthly Board meeting
-

 News5 days ago
News5 days agoRayner and Lammy visit Wales to discuss justice and community safety
-

 News4 days ago
News4 days agoFishguard linked to allegations in Many Tears Animal Rescue investigation
-

 News2 days ago
News2 days agoEmergency services flood Haverfordwest after reports of person in river
-

 Charity7 days ago
Charity7 days agoMany Tears Animal Rescue visited by inspectors as police attend in support role
-

 Local Government5 days ago
Local Government5 days agoInvestigation confirmed after inspectors visit Many Tears Animal Rescue
-

 Crime7 days ago
Crime7 days agoNew rural and wildlife crime strategy aims to boost patrols and community engagement
-

 Community7 days ago
Community7 days agoChoir performs for residents at Kensington Court




























