Health
The NHS at 75: Urgent national dialogue required to address future healthcare needs

AS THE NATION celebrates the 75th anniversary of the NHS, the Welsh NHS Confederation has called upon the Welsh and UK Governments to engage in a comprehensive national conversation regarding the innovation and transformation of the health and care system. In a press release, the Welsh NHS Confederation emphasised the need to adapt to meet the requirements of future generations.
On Wednesday, 5th July, the Welsh NHS Confederation will present a report at the Senedd, signalling the commencement of a public debate on the future of healthcare and care services. The organisation acknowledges the public’s enduring trust in the NHS and its fundamental principles of providing free care to all in need. However, it is widely recognised that the existing health and care services are unsustainable. Over the past 75 years, the demographics of the population have undergone significant changes, with substantial improvements in life expectancy for both men and women in England and Wales, an achievement to be celebrated.
Nevertheless, the challenges posed by an ageing population with increased frailty and chronic conditions necessitate a thorough re-evaluation of health and social care. The NHS is confronted with mounting demands while simultaneously contending with immediate pressures that impede long-term planning for health and care services.
This pivotal moment calls for collaborative efforts to co-produce and redesign services, ensuring they effectively adapt to the evolving needs of the population and remain sustainable in the future. Crucially, the NHS must empower individuals to make informed decisions about their own well-being and independence, guaranteeing access to the most appropriate care for their specific requirements.
It is vital to recognise that access to healthcare represents only a fraction of a population’s overall health, with socio-economic factors playing a substantial role. Wales, for instance, faces the highest poverty rate among the four nations of the UK, with more than one-third of children (34 per cent) living in poverty.
The Welsh population grapples with a multitude of health challenges that hinder life expectancy and widen inequalities, many of which lie beyond the direct purview of the NHS. Improving population health and well-being necessitates an integrated approach that encompasses services and sectors beyond healthcare. Redirecting resources towards long-term investment in public engagement and communication, as well as implementing preventative measures across sectors such as housing, education, transport, and access to the arts and leisure, is imperative. All sectors bear responsibility for creating a preventive model, fostering an economic, social, and natural environment in Wales that supports good health and well-being throughout one’s life.
Continuing along the current trajectory is not an option; change is needed urgently. A transparent and candid conversation with the public about the future of health and care services is essential. This discussion must revolve around an NHS that receives adequate and sustainable funding, an NHS that delivers care and prevention directly to individuals and communities, an NHS that empowers and enables, and one that benefits from improvements in public health. The foundation of this dialogue must be an ambitious and sincere partnership between the NHS and the people it serves.
Darren Hughes, Director of the Welsh NHS Confederation, expressed the importance of adapting to opportunities and challenges, a characteristic deeply ingrained in the NHS’s history. He acknowledged the invaluable contributions of NHS staff, social care staff, volunteers, third-sector organisations, unpaid carers, and communities in supporting the nation’s health and well-being. However, Hughes cautioned that the existing efforts alone are insufficient to ensure the long-term sustainability of health and care services for future generations. He emphasised the urgency of engaging in a national conversation to unite behind a shared vision for the NHS’s future. Hughes highlighted that the responsibility lies with the population and all sectors
Health
Doctors say Wales is failing to value NHS staff over new pay award

BMA Cymru Wales accuses ministers of falling short on pay restoration as Welsh Government accepts DDRB recommendations for 2026-27
DOCTORS in Wales have accused the Welsh Government of failing to properly value NHS staff after ministers accepted this year’s independent pay recommendations for medical and dental professionals. The row centres on whether the award represents fair recognition for frontline staff — or yet another missed chance to reverse years of falling real-terms pay.
In a written statement published on Wednesday (Mar 25), Health Secretary Jeremy Miles said the Welsh Government had accepted the Doctors’ and Dentists’ Review Body recommendations on headline pay for 2026-27. Under the decision, consultants, specialty and associate specialist doctors, resident doctors, dentists and locally employed doctors will receive a 3.5% consolidated uplift from April 1, 2026, while salaried dentists in Community Dental Services and the Public Dental Service will receive 3.75%.
But while the Welsh Government also said it accepted in principle a 3.5% uplift for contractor GPs and a 3.75% uplift to the pay element of dental contracts, ministers made clear that final decisions on how those increases are applied alongside wider contract changes would be left to the next government.
That has triggered an angry response from BMA Cymru Wales. In a press release issued on Wednesday, Dr Iona Collins, chair of the BMA’s Welsh Council, said ministers had “once again chosen to impose an award that falls short” of repeated promises to deliver full pay restoration for doctors employed by NHS Wales.
She said the award failed to reflect the “superhuman” efforts of doctors working under intense pressure and warned that inadequate pay would make it harder to retain staff in the Welsh NHS at a time when many are considering leaving for better pay and conditions elsewhere.
The BMA also raised concerns about general practice, saying GP pay had effectively been left hanging because the Cabinet Secretary linked the award to ongoing General Medical Services contract discussions with the incoming administration. The union said this left general practice “out in the cold” compared with other branches of the profession and called for urgent talks.
The Welsh Government said the award would apply from April 1 and added that wider DDRB recommendations not directly related to headline pay would be considered separately with partners. Ministers thanked NHS staff for their “ongoing dedication and hard work”.
The dispute is likely to reignite the wider argument over recruitment, retention and morale in NHS Wales, with doctors’ leaders insisting that pay restoration is no longer simply about reward, but about preventing more clinicians from walking away from the service.
Health
Same Day Emergency Care unit at Glangwili to reopen after £2m refurbishment
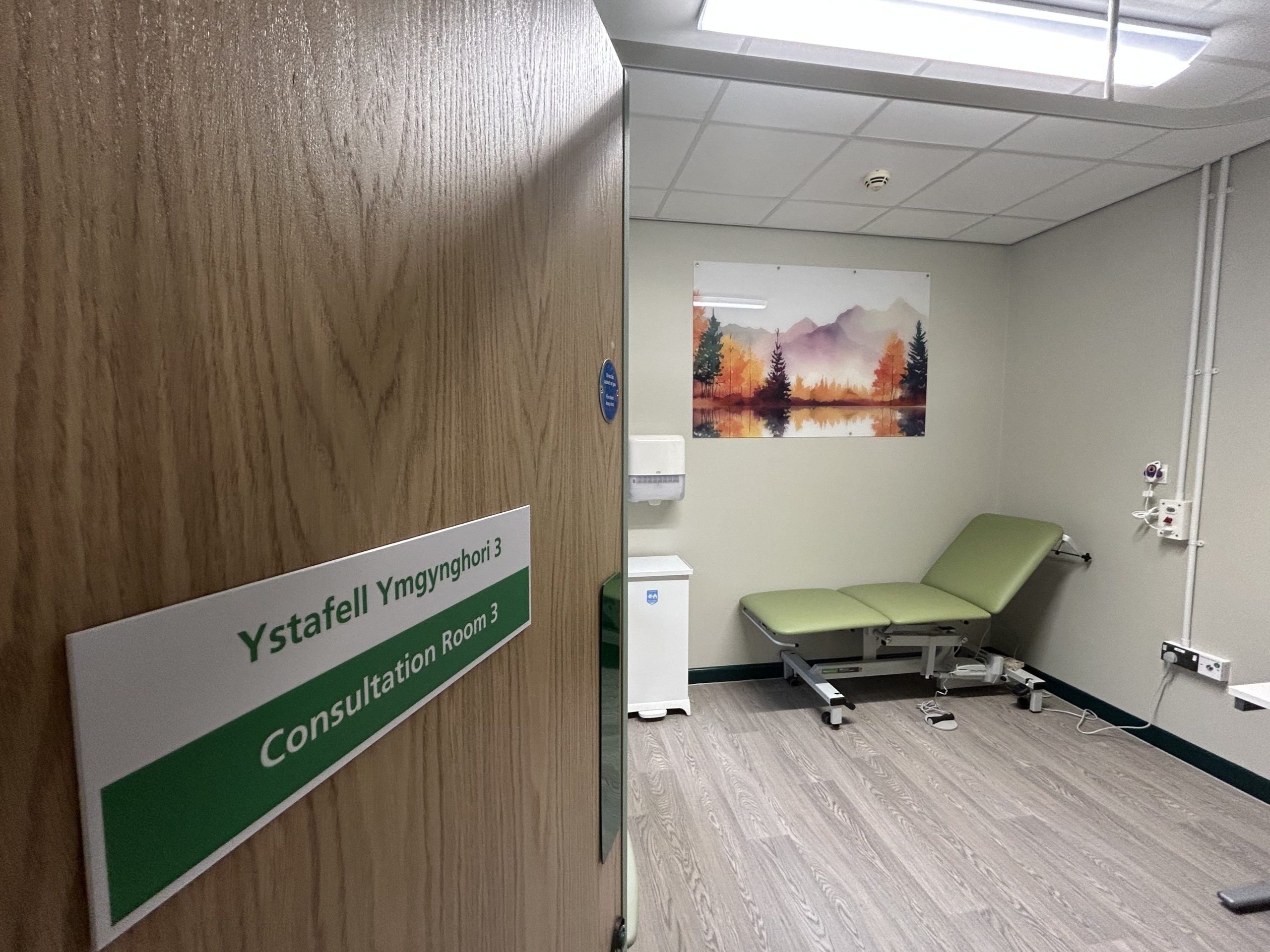
THE SDEC unit at Glangwili Hospital in Carmarthen will reopen to patients and staff on Monday (Mar 30) following a major £2m refurbishment.
The upgrade, funded by the Welsh Government, has delivered additional consultation rooms, a redesigned reception area, and improved facilities aimed at enhancing the experience for both patients and staff.
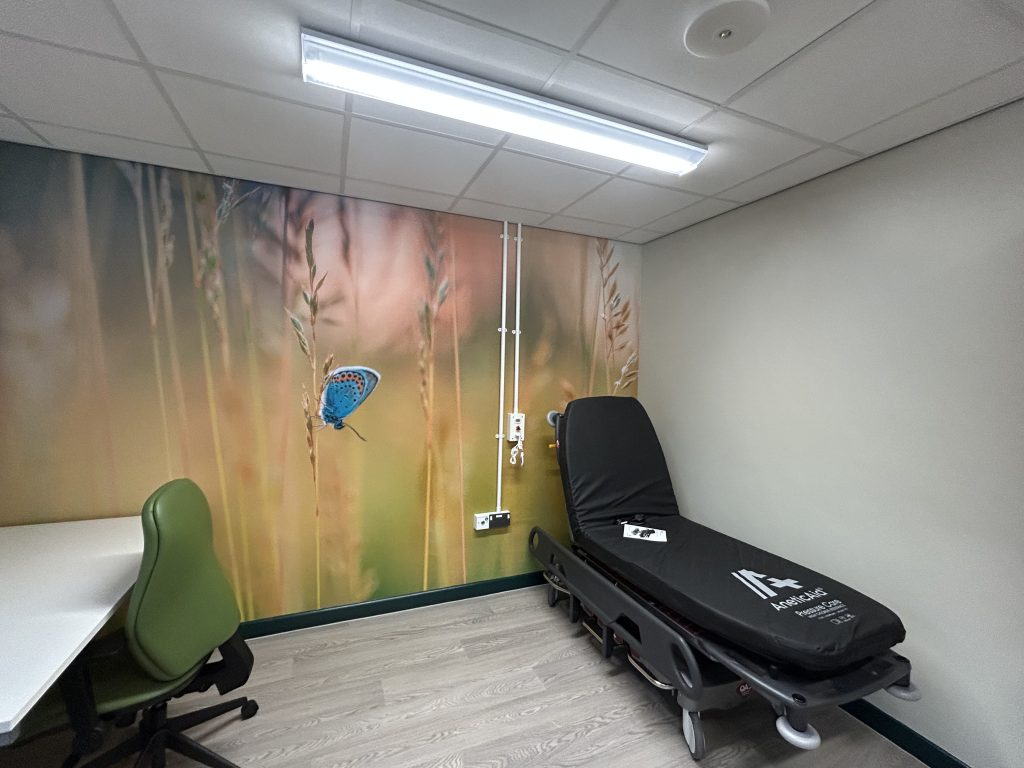
Health board chiefs say the revamped unit is expected to ease pressure on the hospital’s Emergency Department and forms part of wider efforts to improve urgent care services across Hywel Dda University Health Board sites, including the Minor Injury Unit at Prince Philip Hospital.

Keith Jones, Director of Operational Planning and Performance at Hywel Dda, said: “We are very grateful to the Welsh Government for the £2.096 million investment, which has allowed us to increase capacity within the SDEC unit at Glangwili.
“We expect these improvements will help reduce pressure on the Emergency Department and enable our teams to deliver a smoother, faster experience for patients.”
During the works, several services were temporarily relocated to Y Lolfa, formerly Padarn Ward. These will now return to the SDEC building, including the Discharge Lounge, Medical Day Unit and the Primary Care Out of Hours Service.
Cancer support services, including the Cancer Information and Support Service (CISS) and Cancer Psychological Support Service (CaPS), will also move back to the unit.
Access routes for services that remained at the Priory Day Hospital during the refurbishment – including podiatry, neuro-rehabilitation and occupational therapy – will return to normal.
Patients are advised to follow on-site signage or ask staff for directions. The health board said appointment letters will include updated information, but urged patients to double-check details and contact departments directly if unsure.
Mr Jones added: “I would like to thank staff, patients and visitors for their patience during these works.”
Cabinet Secretary for Health and Social Care Jeremy Miles said the investment would deliver “real improvements” for patients and staff.
He added: “This is part of our ongoing commitment to improving hospital facilities across Wales, ensuring people receive the right care, in the right place, as quickly as possible.”
Health
Cervical cancer prevention drive stepped up across Wales

Home testing and vaccine catch-up plan launched as uptake falls after pandemic
PLANS to boost cervical cancer prevention across Wales have been set out by ministers, amid concerns that HPV vaccination rates have fallen since the pandemic.
In a written statement issued on Wednesday (Mar 25), Health Secretary Jeremy Miles said urgent work is underway to improve uptake of both vaccination and screening, which are key to preventing the disease.
The Welsh Government confirmed that before COVID-19, HPV vaccine uptake was close to the World Health Organisation’s 90% target — but levels have since dropped.
Health board vaccination teams have delivered more than 1,400 additional HPV vaccinations during 2025 as part of targeted efforts, particularly focusing on schools where uptake is lowest. Further catch-up programmes are planned over the next 12 months.
Public Health Wales has also launched surveys aimed at understanding why some young people and parents are not attending vaccination appointments, alongside a wider communications campaign highlighting the benefits of the vaccine.
Cervical screening, which detects high-risk strains of HPV, remains a key part of prevention efforts. However, participation varies across different groups.
A new initiative will see at-home cervical screening kits introduced later this year, aimed at women who rarely or never attend appointments. The move is designed to remove barriers to screening and improve access.
Latest figures show a gradual decline in cervical cancer cases and deaths in Wales. The number of cases has fallen from an average of 164 per year in the early 2000s to 149 in recent years, while annual deaths have dropped from 61 to 54.
Despite this progress, ministers say more must be done to improve early detection and treatment.
Cervical cancer is currently grouped within wider gynaecological cancers for NHS treatment targets, but plans are in place to report more detailed data by April 2027 to better track treatment times.
Jeremy Miles urged those eligible to take up both vaccination and screening offers, adding that improving access to prevention, diagnosis and treatment would be key to reducing cancer rates further in the years ahead.
-

 Health7 days ago
Health7 days agoNHS waiting list falls — but cancer delays and diagnostic backlog worsen
-

 Crime6 days ago
Crime6 days agoPembroke man remanded in custody over knife threat, assault and damage allegations
-

 Crime7 days ago
Crime7 days agoIllegal workers found at Cardigan takeaway after immigration raid
-

 Crime5 days ago
Crime5 days agoBroad Haven man remanded in custody over sexual harm prevention order breach
-

 Education6 days ago
Education6 days agoMilford Haven school plans unveiled but funding not yet secured
-

 News7 days ago
News7 days agoCouncil unveils plans for new state-of-the-art secondary school in Milford Haven
-

 Farming7 days ago
Farming7 days ago£3 million secured to continue Welsh sheep genetics programme
-

 Community6 days ago
Community6 days agoFormer Neyland police officer Louis Knight dies aged 83






























