Health
Monkeypox Q&A: how do you catch it and what are the risks? An expert explains
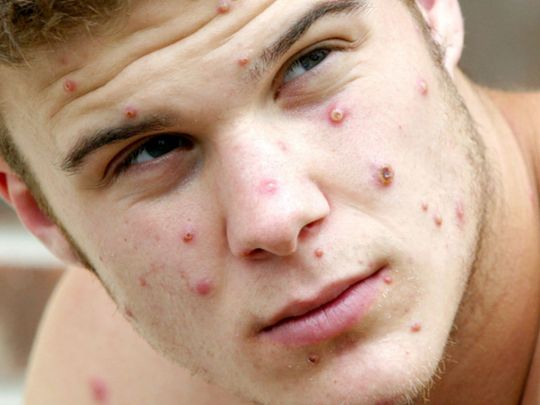
THE LATEST outbreak of monkeypox has, at the time of writing, reached 17 countries with 110 confirmed cases and a further 205 suspected cases. It’s a fast-moving story, so if you need to catch up on the latest, here are answers to some of the most pressing questions.
How is monkeypox spreading?
The first patient in the current outbreak had returned to the UK from travels to Nigeria where monkeypox is endemic. However, cases are now spreading among people who have not travelled to west or central Africa, suggesting local transmission is occurring.
Monkeypox usually spreads by close contact and respiratory droplets. However, sexual transmission (via semen and/or vaginal fluid) has been posited as an additional possible route. The World Health Organization (WHO) says: “Studies are needed to better understand this risk.”
Most cases in the current outbreak have been in youngish men, but the virus can spread to anyone.
There are no confirmed cases in Pembrokeshire at the present time.
What are the symptoms?
Early symptoms are flu-like, such as a fever, headaches, aching muscles and swollen lymph nodes.
Once the fever breaks, a rash can develop, often beginning on the face and then spreading to other parts of the body – most commonly the palms of the hands and soles of the feet.
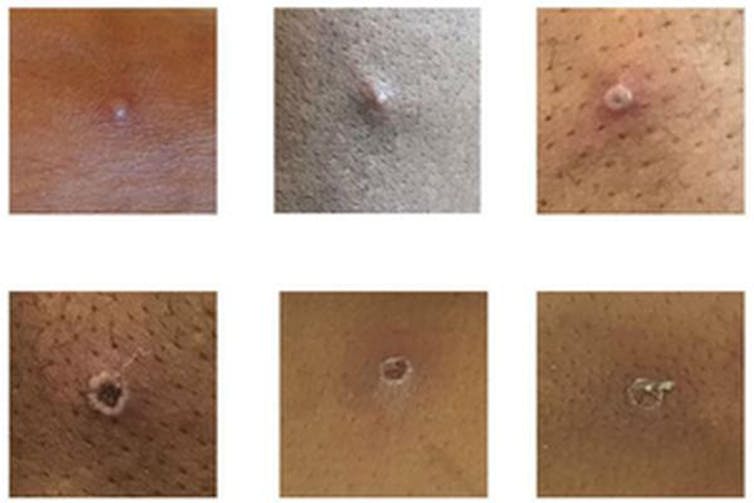
How deadly is monkeypox?
Monkeypox is mostly a mild, self-limiting disease lasting two-to-three weeks. However, in some cases, it can cause death. According to the WHO, the fatality rate “in recent times” has been around 3% to 6%. The west African monkeypox virus is considered to be milder than the central African one.
Monkeypox tends to cause more serious disease in people who are immunocompromised – such as those undergoing chemotherapy – and children. There have been no deaths from monkeypox in the current worldwide outbreak, but, according to the Daily Telegraph, one child in the UK is in intensive care with the disease.
Why is it called monkeypox?
Monkeypox was first identified in laboratory monkeys (macaques) in Denmark in 1958, hence the name. However, monkeys don’t seem to be the natural hosts of the virus. It is more commonly found in rats, mice and squirrels. The first case in humans was seen in the 1970s in the Democratic Republic of the Congo.
Is monkeypox related to smallpox and chickenpox?
Monkeypox is related to smallpox – they are both orthopoxviruses – but it is not related to chickenpox. Despite the name, chickenpox is a herpes virus, not a poxvirus. (How “chicken” got in the name is not entirely clear. In his dictionary of 1755, Samuel Johnson surmised that it is so named because it is “of no very great danger”.) Nevertheless, the vesicles (little pus-filled blisters) caused by monkeypox are similar in appearance to those of chickenpox.
Are cases likely to continue rising?
Cases are likely to continue to rise significantly over the next two-to-three weeks, but this is not another pandemic in the making. Monkeypox doesn’t spread anywhere near as easily as the airborne virus SARS-CoV-2 that causes COVID-19.
Has monkeypox evolved to be more virulent?
RNA viruses, such as SARS-CoV-2, don’t have the ability to check their genetic code for mistakes each time they replicate, so they tend to evolve faster. Monkeypox is a DNA virus, which does have the ability to check itself for genetic mistakes each time it replicates, so it tends to mutate a lot slower.
The first genome sequence of the current outbreak (from a patient in Portugal) suggests that the virus is very similar to the monkeypox strain that was circulating in 2018 and 2019 in the UK, Singapore and Israel. So it is unlikely that the current outbreak is the result of a mutated virus that is better at spreading.
How is monkeypox diagnosed?
In the UK, swab samples taken from the patient are sent to a specialist laboratory that handles rare pathogens, where a PCR test is run to confirm monkeypox. The UK Health Security Agency has only one rare and imported pathogens laboratory.
Is there a vaccine for it?
Vaccines for smallpox, which contain the lab-made vaccinia virus, can protect against monkeypox. However, the vaccine that was used to eradicate smallpox can have severe side-effects, killing around one in a million people vaccinated.
The only vaccine specifically approved for monkeypox, Imvanex, is made by a company called Bavarian Nordic. It uses a nonreplicating form of vaccinia, which causes fewer side-effects. It was approved by the US Food and Drug Administration and the European Medicines Agency in 2019 – but only for use in people 18 years of age or older.
UK health secretary Sajid Javid said that the UK government will be stocking up on vaccines that are effective against monkeypox. The UK currently has about 5,000 doses of smallpox vaccine, which has an efficacy of around 85% against monkeypox.
Are there drugs to treat it?
There are no specific drugs to treat monkeypox. However, antivirals such as cidofovir and brincidofovir have been proven to be effective against poxviruses in animals and may also be effective against monkeypox infections in humans.
By Ed Feil, Professor of Microbial Evolution at The Milner Centre for Evolution, University of Bath
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Health
FOI raises fresh questions over plan to close Pontyates GP surgery

Health board accused of misleading claims over recruitment as pressure mounts ahead of final decision
A FREEDOM of Information disclosure has raised serious questions over plans to close Meddygfa’r Sarn in Pontyates, with claims the health board failed to properly attempt to recruit permanent doctors before recommending its shutdown.
The row centres on Hywel Dda University Health Board, which is due to make a final decision on the surgery’s future later this month.
An FOI response reveals that while the board cited a “lack of recruitment interest” in its January report, there is limited evidence of any recent, targeted recruitment campaign specifically aimed at the Pontyates practice.
Instead, the board confirmed that salaried GP roles were advertised in 2020 across its wider portfolio of managed practices — rather than as a focused effort to fill posts at Meddygfa’r Sarn itself. Those vacancies did not result in successful appointments.
‘No real attempt’
Independent Senedd candidate Carl Peters-Bond, who is also a patient at the surgery, has strongly criticised the health board, accusing it of presenting a misleading picture to justify closure.
He said: “They cited a lack of recruitment interest as justification for closing this surgery — but they never actually ran a proper recruitment campaign for it.
“Sending out general adverts years ago is not the same as making a serious, targeted effort to keep a vital community service alive.”
He also raised concerns about the consultation process, claiming it focused on the impact of closure rather than asking whether closure should happen at all.
Fully reliant on locums
The FOI confirms that Meddygfa’r Sarn currently has no salaried GPs and is entirely dependent on locum doctors.
While the health board says this model is unsustainable in the long term, the same disclosure shows several other managed practices across the region also rely heavily on locum staff — some to a significant degree.
Cost data included in the response suggests Meddygfa’r Sarn is not the most expensive practice per patient within the health board’s area.
Alternative options unclear
Another key issue raised by campaigners is the apparent lack of explored alternatives.
The FOI response indicates that the health board does not hold information on alternative local solutions, including potential relocation or different service models within the Pontyates area.
Campaigners argue this suggests closure was considered before all options had been properly examined.
A 52-page independent report submitted as part of the consultation process states that dispersing patients to other surgeries should only be considered as a last resort, after full recruitment efforts and capacity assessments have been carried out.
Health board position
Hywel Dda University Health Board maintains that the surgery, which serves around 4,350 patients, has faced long-standing recruitment difficulties and increasing reliance on temporary staff.
It says a Vacant Practice Panel concluded that dispersing patients to neighbouring surgeries would provide a more sustainable long-term solution.
The board has also acknowledged that transport and access concerns are likely to be a major issue for patients if the closure goes ahead, with a full Equality Impact Assessment expected to be considered before a final decision.
Decision later this month
The future of Meddygfa’r Sarn will be decided at a meeting of Hywel Dda University Health Board on Wednesday (May 28) at Yr Egin in Carmarthen.
With local anger growing and new questions emerging from the FOI disclosure, pressure is mounting on board members to reconsider the proposal.
Campaigners say the case now hinges on a simple question: whether enough was done to save the surgery before moving to close it.
Health
Turkish dental clinic to hold Haverfordwest meet-up
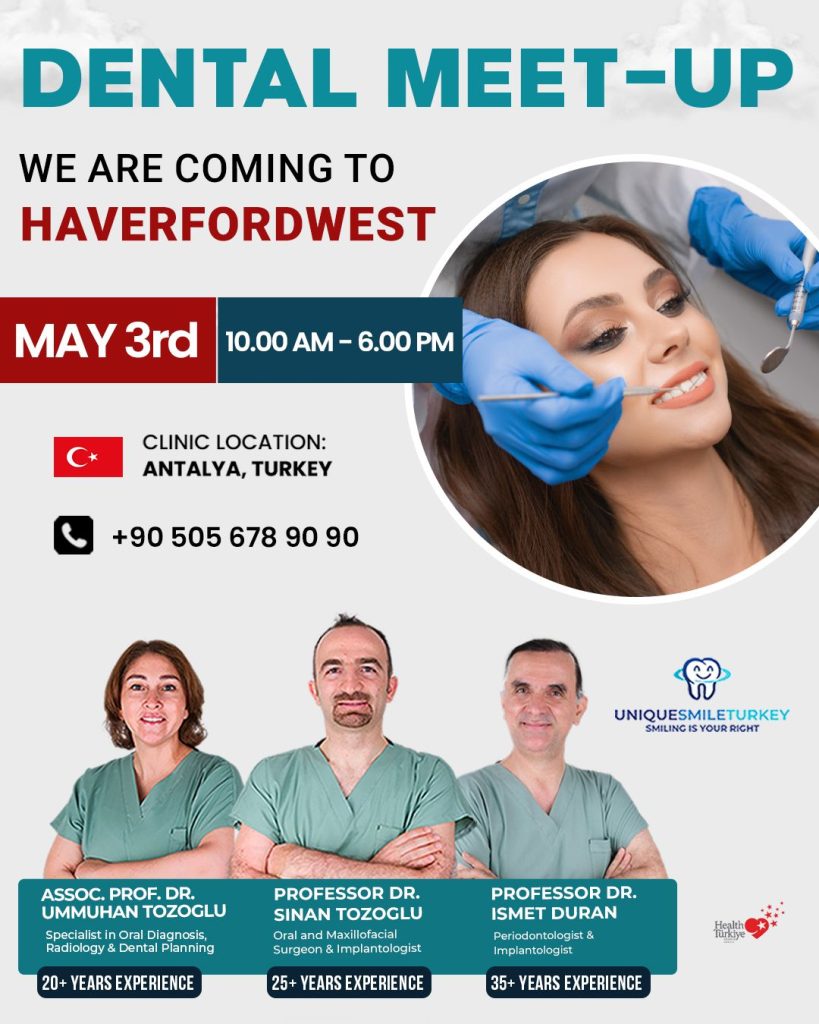
DENTISTS FROM ANTALYA TO VISIT COUNTY TOWN
A TURKISH dental clinic is running a dental meet-up in Haverfordwest this weekend as part of a promotional visit to Wales.
Unique Smile Turkey, which has a permanent office in Wales in Swansea, says its top dentists will be coming to Haverfordwest on Sunday (May 3).
The event is being advertised as a “Dental Meet-Up” and is scheduled to run from 10:00am to 6:00pm at the Mariners Hotel.
The visit features three clinicians: Assoc Prof Dr Ummuhan Tozoglu, described as a specialist in oral diagnosis, radiology and dental planning; Professor Dr Sinan Tozoglu, described as an oral and maxillofacial surgeon and implantologist; and Professor Dr Ismet Duran, described as a periodontologist and implantologist.
The team have between twenty and 35 years of experience in their respective fields.
A contact number has also been provided for enquiries: +90 505 678 90 90.
The visit comes amid continuing interest in dental tourism, with many people in the UK looking overseas for cosmetic dentistry, implants and other private dental treatment.
Turkey has become one of the most popular destinations for such treatment, although patients are generally urged to make careful checks before committing to any procedure abroad, including aftercare arrangements, qualifications, insurance, treatment plans and what support would be available if complications arise after returning home.
Health
Welsh public backs urgent action on dementia ahead of Senedd elections

Calls grow for diagnosis, care and support to become national priority
NEW figures reveal overwhelming public demand for dementia to be placed at the top of Wales’ political agenda, with voters urging action on diagnosis, treatment and support ahead of the Senedd elections.
Research by Alzheimer’s Society Cymru shows that 83% of people in Wales want dementia made a healthcare priority, while 69% believe it is currently overlooked and underfunded.
More than a thousand adults were surveyed, with the findings highlighting growing concern over diagnosis rates and access to care. Wales continues to record some of the lowest dementia diagnosis rates in the UK, leaving thousands of families without clarity or support.
Around 51,000 people are currently living with dementia in Wales, a figure expected to rise to 70,000 by 2040. Despite this, only 57% of people have received a formal diagnosis, with rates falling as low as 48% in rural areas such as Powys.
Improving diagnosis remains a key concern, with 91% of those surveyed saying access to timely diagnosis must improve, and 87% backing increased investment in diagnostic services. However, respondents also stressed that diagnosis alone is not enough, with 91% saying people with dementia must receive better support, including help for unpaid carers.
Ceri Parry, from Cardiff, said she was forced to retire early from her role as a headteacher at the age of 55 due to a lack of support for her mother, who was diagnosed with Alzheimer’s disease in 2020.
She said: “I fully support improving early and accurate diagnosis, but this must also come with improved support and care for families afterwards. There’s five years between my relatives’ diagnoses and nothing changed. On both occasions we left with a leaflet and the unknown.
“The wait for improved diagnosis, treatment and support needs to end. Dementia must be a top priority for the next Welsh Government, for families living with it now and for those who will face it in the future.
“We also found there was no diagnosis assessment available in the Welsh language. That’s a fundamental issue if a diagnosis is to be accurate and safe for people who speak Welsh as their first language. Ignoring someone’s identity is ignoring the person.”
The survey also found that visible action would be key to restoring public confidence, with 72% calling for improved dementia services, 64% backing more funding for research, and 63% wanting better access to treatments.
Gemma Roberts, National Influencing Manager at Alzheimer’s Society Cymru, said: “Dementia is Wales’s biggest killer and one of the greatest health and social care challenges we face.
“Hope is on the horizon with new treatments and faster, more accurate diagnosis, but the system is not keeping pace. Without urgent transformation, people in Wales risk missing out.
“We are at a turning point. The next Welsh Government must deliver a bold new dementia strategy that transforms diagnosis and ensures access to quality care, treatments and support.”
-

 News19 hours ago
News19 hours agoBaby in critical condition after Fishguard emergency
-

 Community6 days ago
Community6 days agoDogs removed after welfare concerns at Milford Haven property
-

 Crime7 days ago
Crime7 days agoPembrokeshire hairdresser avoids prison after pub assault
-

 Crime7 days ago
Crime7 days agoPembrokeshire man charged with making hundreds of indecent images of children
-

 Business7 days ago
Business7 days agoHandcrafted garden furniture built to last across Pembrokeshire
-

 Charity7 days ago
Charity7 days agoRow erupts at Spitfire museum after Reform poster displayed at charity premises
-

 Community7 days ago
Community7 days agoCancer patients targeted with parking fines outside Haverfordwest support centre
-

 Community2 days ago
Community2 days agoTenby phone signal crisis goes national as businesses warn of summer disruption



























