Health
St Davids Surgery will close despite strong opposition, residents told

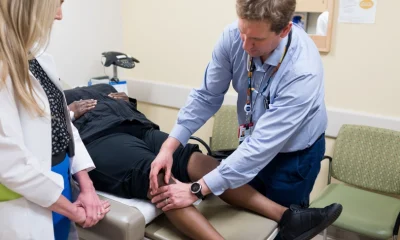
HYWEL DDA has confirmed the closure of St Davids Surgery this week, dismissing widespread local opposition and calls for reconsideration. This decision follows a packed public meeting where residents voiced their concerns about the loss of the vital healthcare facility.
The announcement to close the surgery was made in July, with the health board revealing that the surgery would shut down next month when its only GP resigns from the General Medical Services contract. Around 3,000 patients are registered at the surgery and will now be transferred, mainly to Solva Surgery, with others sent to Fishguard and Haverfordwest surgeries depending on their location.
This decision sparked significant backlash from the local community. A drop-in session held at City Hall saw hundreds of St Davids residents lining up outside the doors to express their concerns directly to the health board. Protest banners sprang up around the city, highlighting the depth of public feeling against the closure.
Undeterred, the residents of St Davids have continued their efforts to save the surgery.
Last week, more than 150 people gathered at City Hall for a meeting to discuss possible next steps. Topics included appealing the health board’s decision and exploring the option of the community purchasing the surgery building.

Despite the strong local campaign, the health board has stated it will not reconsider its decision. In a letter to campaigners, it acknowledged the concern and disappointment caused but confirmed that a branch surgery will be set up in St Davids. This new branch will offer services from a multi-professional team for a minimum of 20 hours per week but will not include any sessions run by a physician associate, limiting support for doctors in patient care.
The health board plans to begin the patient transition process in the coming weeks. The management team is collaborating with staff at both St Davids Surgery and Solva Surgery to develop a new model of general practice. This model aims to meet the health board’s statutory requirement to provide appropriate services for St Davids residents by the end of October.
Hywel Dda Health Board has expressed its commitment to ongoing cooperation with the Peninsular Working Group. It has also pledged to review the general medical services (GMS) provision in six months to ensure it continues to meet patients’ needs. In addition, health board engagement events on the development of primary and community services strategy are scheduled throughout September.
Dr Neil Wooding, the newly appointed chairperson of Hywel Dda University Health Board, and acting CEO Prof Phil Kloer addressed the decision: “In making the decision to support the managed list dispersal of the current St Davids Surgery, members of the board were presented with all of the facts related to patient demographics, travel times, etc. This also included discussions with the current owners of the surgery building, Llais, and the local medical committee.”
“We will not revisit this decision but will continue to work with the community of St Davids to mitigate any negative impact of this development where possible,” they added.
While the health board remains firm in its decision, the residents of St Davids are determined to keep fighting for local healthcare services, hoping to minimise the impact of the surgery’s closure on their community.
Health
Patients in Wales waiting years for autoimmune diagnosis
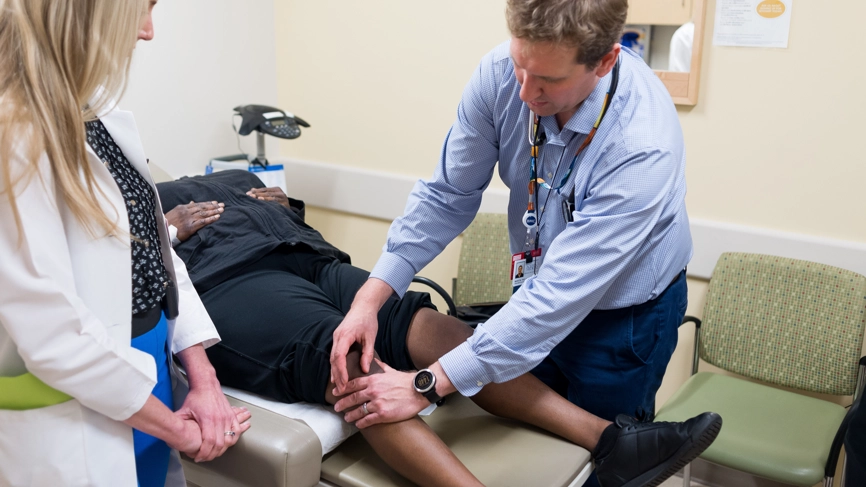
Study led by Swansea University says long delays, limited specialist access and referral barriers are leaving some patients worse off than those elsewhere in the UK
PEOPLE in Wales with autoimmune and rheumatological conditions are facing long waits for diagnosis, poor access to specialist care and repeated obstacles when trying to secure treatment outside their local area, according to new research.
The study, led by Swansea University, examined the experiences of patients with illnesses including lupus and other autoimmune disorders. It drew on interviews, survey findings and Freedom of Information responses from health boards across Wales.
Researchers found that specialist provision remains limited in some parts of the country. Some patients reported having no access to a lupus specialist in their area, while FOI responses indicated there is only one NHS neuro-ophthalmologist in Wales for patients with neurological or visual problems linked to autoimmune disease.
The report also highlighted a lack of diagnostic services. None of the Welsh health boards that responded said they currently provide nailfold capillaroscopy, a test used to help identify conditions such as scleroderma.
Diagnosis in rheumatology can also be difficult because many of the conditions involved are complex and may develop gradually over time. Illnesses such as ankylosing spondylitis can be mistaken in the early stages for more common causes of pain, while autoimmune disorders often present with symptoms that overlap with other conditions.
Patients may require a combination of investigations before a diagnosis can be confirmed, including HLA-B27 testing, routine blood work, MRI scans, X-rays and detailed clinical assessment. Doctors also rely heavily on patient interviews to build up a picture of pain, stiffness, mobility and the wider pattern of symptoms.
There have also been local pressures on services in west Wales. At Withybush Hospital, delays were caused after the departure of a specialist consultant, and it took some time for that post to be filled. That consultant has now been replaced. However, it is understood the workload remained heavy, with the specialist working through a backlog of cases.
In some cases, patients may also feel rheumatology is treated as a lower-profile service. At Withybush Hospital, for example, the department has been based in a portacabin in the hospital car park, which it shares with the lymphoedema service — a setting that can give the impression that two important but often overlooked specialties are being accommodated on the margins of the wider hospital system.
Rheumatology also places a significant burden on the NHS because of the cost of long-term treatment and follow-up care, although that is not the main focus of the study. Biological drugs used to treat conditions such as rheumatoid arthritis and ankylosing spondylitis can cost around £500 for a pack of four injections, according to local hospital sources. Patients on those medications often also require regular blood monitoring, consultant reviews, specialist nurse support and physiotherapy. The Herald understands that more than 1,000 patients in Pembrokeshire are currently being managed through this treatment pathway.
Researchers said patients were also being held back by the referral system. Under current NHS Wales rules, doctors must apply to their local health board for permission to send patients for treatment outside the area or across the border into England. The study said decision-making around those requests was often inconsistent and unfair.
One patient with systemic lupus erythematosus told researchers he waited two years for approval to be referred to England, despite believing the process should only have taken weeks.
The study found that patients in Wales often face longer journeys to diagnosis than elsewhere in the UK. In the sample reviewed by researchers, the average time from first symptoms to diagnosis was around 11 years, compared with around seven years across the UK.
Patients described the effect those delays had on their health. One woman in her 30s said requests to see a specialist in a neighbouring health board had been turned down, and that her lupus had worsened as a result. Another patient said access to care became more difficult after moving from England to Wales.
The research was led by Rupert Harwood of Swansea University Medical School, who himself lives with several autoimmune conditions.
His own experience reflects the wider concerns raised in the report. After developing visual symptoms in 2016, he was advised to see a neuro-ophthalmologist, but no such service was then available in Wales. A referral to England was not successfully made until 2025, and he is still waiting for an appointment.
Mr Harwood said the present system can leave patients at a disadvantage if they cannot afford to seek private treatment outside Wales.
The study concludes that while NHS Wales rheumatology teams provide high-quality care, patients in Wales face additional barriers compared with those in England.
Researchers are calling for a review of the out-of-area referral system, better access to specialist services and greater investment in diagnostic testing to reduce delays and improve outcomes.
Health
Lib Dems vow to keep Palantir out of Welsh public services

Party says it would use its influence in the next Senedd to block any move to bring the firm into the NHS or government systems in Wales
THE Welsh Liberal Democrats have pledged to use their influence in the next Senedd to keep controversial technology firm Palantir out of Wales’ NHS and wider public services.
The party said it would oppose any attempt to introduce the company into Welsh Government systems, citing concerns over data security, transparency and Palantir’s wider links to military and intelligence work.
The move comes amid increasing scrutiny of Palantir’s £300m contract with NHS England and reports that UK ministers are considering whether to activate a break clause.
The Welsh Liberal Democrats said Wales must not follow what they described as a risky approach to the handling of sensitive public data.
A debate on the issue is due to be led in Westminster today by Liberal Democrat MP Martin Wrigley.
The party said it supported better data integration to improve patient care and help reduce waiting times, but argued that this should not come at the expense of public trust or national security.
Instead, the Lib Dems are calling for investment in what they describe as trusted and transparent alternatives, including British-based providers, to modernise digital infrastructure without raising concerns over foreign influence or the handling of personal data.
The party also said that, in a finely balanced Senedd, it would use its votes to block any effort to bring Palantir into Welsh public services.
It warned that once contracts involving critical digital systems are signed, they can be difficult to reverse, and said ministers in Wales should take a precautionary approach now rather than try to solve problems later.

Commenting, Welsh Liberal Democrat Westminster spokesperson David Chadwick MP said: “People across Wales will rightly be asking why a controversial foreign tech company with links to military and intelligence operations is being trusted with something as sensitive as our health data.
“The Welsh Liberal Democrats are clear: Palantir should be nowhere near our NHS or our public services. Trust in how data is handled is absolutely fundamental, and once that trust is lost, it is incredibly difficult to rebuild.
“In the next Senedd, we will use our votes to make sure this company is kept out of Wales. There can be no compromise when it comes to protecting people’s personal information and safeguarding our national security.
“We all want to see better joined-up care, shorter waiting lists and a modern NHS fit for the future. But that must be delivered in a way that puts patients first, not by handing over the keys to organisations that many people simply do not trust.
“Wales should be leading the way in building secure, transparent digital systems that the public can have confidence in, not going down a path that risks undermining that trust.”
Health
Tracy’s firewalk raises £528 for Withybush rheumatology unit

Long-serving staff member and patient took on 800°C embers to give back to service that has supported her family for years
A MEMBER of staff at Withybush Hospital has raised £528 for Rheumatology Services after taking part in Hywel Dda Health Charities’ firewalk challenge.
Tracy Beynon, who has worked at Withybush for 23 years and has also been a rheumatology patient for 20 years, took part in the barefoot walk across 800°C embers in October to support the department.
She said she had always wanted to try a firewalk and jumped at the chance to do one for her local health board.
Tracy said: “Over the years, I have done some wild things to raise money for various charities, including shaving my head after a Six Nations rugby match 11 years ago.
“Rheumatology have looked after many generations of my family throughout the years, and I wanted to try and give something back to help the team and the patients they serve.
“I was stunned by how much money I raised. After I put a video on TikTok, I had a number of donations from people I have never even met. I will forever be thankful to my friends and family for supporting all of my mad fundraising ideas.”
Katie Hancock, Fundraising Officer for Hywel Dda Health Charities, said: “A huge thank you to Tracy for showing her support to the service that has taken such good care of her for so long.
“The generous charitable donations we receive do not replace NHS funding. Instead, they support additional items and activities outside core NHS expenditure. These small extras make a big difference, and we are so grateful for every donation we receive.”
Hywel Dda Health Charities said donations help provide added items and activities for local NHS patients and staff beyond core NHS spending.
For more information about the charity and how to support local NHS services, visit the Hywel Dda Health Charities website.
-

 Business5 days ago
Business5 days agoA proper Pembroke local: Inside the warm welcome of The Old Cross Saws Inn
-

 Sport6 days ago
Sport6 days agoGrand Slam win for Pembrokeshire rugby ace
-

 Business3 days ago
Business3 days agoMilford Haven dry dock pitched as home for giant £480m superyacht yard
-

 Community5 days ago
Community5 days agoDoorstep warning issued after reports of suspicious callers in Pembrokeshire
-

 Crime5 days ago
Crime5 days agoRomino’s licence revoked after illegal workers found and fire risks exposed
-

 Politics4 days ago
Politics4 days agoWelsh Lib Dems promise childcare boost, social care reform in manifesto launch
-

 Business7 days ago
Business7 days agoPlans submitted to add gym and café to ferry terminal
-

 News5 days ago
News5 days agoTrump image row sparks attack from Eluned Morgan